For Your Healthcare Provider
Have your patient scan this QR code with their smartphone camera to instantly access this educational guide on their device.

A guide for patients with a low lymphocyte count
Access the Resources
Note: The video and audio linked above were generated with the assistance of AI. Clinical accuracy has been reviewed, but no AI-generated content can be guaranteed to be fully error-free.
A low lymphocyte count can be unsettling when you first see it on a blood test, especially if you are not sure what lymphocytes do or why the number matters.
Lymphocytopenia is common and usually temporary, often occurring during or after infections, illness, stress, or certain medications. It does not mean cancer or a failing immune system. Most people feel well, and the count often returns to normal on its own. Your doctor will explain what your number means, why follow-up matters, and how monitoring keeps you safe.
This guide is for people with a low lymphocyte count found in outpatient or non-emergency settings; it does not apply to severely ill or hospitalized patients, immune emergencies, or rapidly falling blood counts.
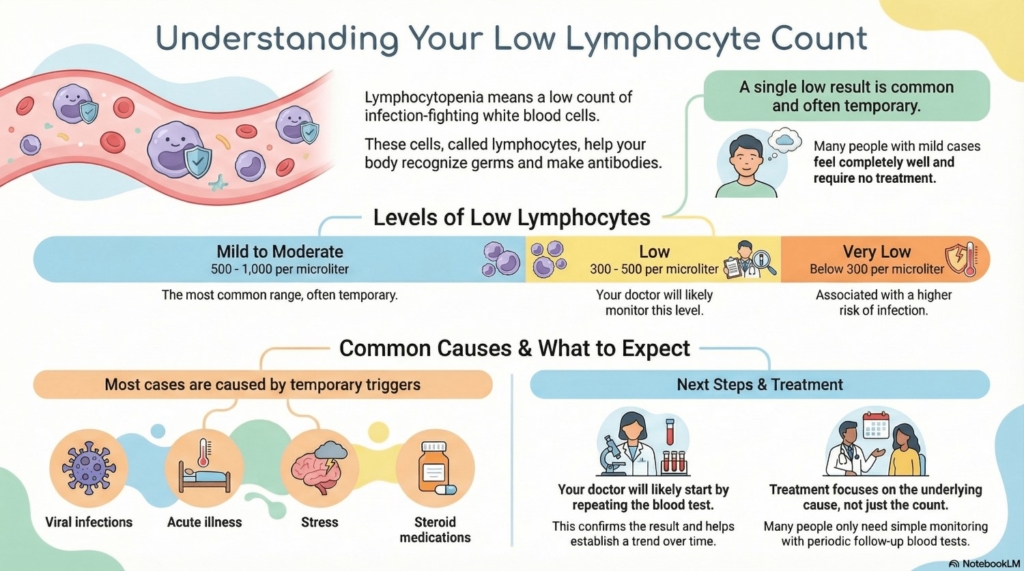
First things first
Many people discover this result while reviewing their CBC online. Mild lymphocytopenia usually reflects infection, illness, stress, or medications, and most people feel completely well.
A single low result often improves on its own. Your doctor will guide whether any follow-up is needed.
What are lymphocytes?
Lymphocytes are white blood cells that help protect you from infections. They allow your body to:
- recognize germs
- make antibodies
- “remember” infections for faster protection in the future
Three major types exist (B cells, T cells, NK cells), but the CBC groups them together as “lymphocytes.”
What is lymphocytopenia?
Lymphocytopenia means your lymphocyte count is lower than the laboratory’s reference range.
Helpful context:
- lymphocytes help your body fight infections
- many people with mild lymphocytopenia feel completely well
- a single low result is common and often temporary
How lymphocytes are measured
Lymphocytes are part of the CBC with differential.
Most adults have:
- 1,000–4,000 lymphocytes per microliter
A value below 1,000 is considered lymphocytopenia in most adults.
Your CBC may report lymphocytes as:
- “×10⁹/L”
- “K/µL”
Both represent the same quantity.
Ranges that matter
- mild lymphocytopenia: 800–1,000
- moderate: 500–800
- low: 300–500
- very low: <300 (higher infection risk)
Mild decreases are common, especially during illness or stress.
Why it happens (causes)
Temporary causes (most common)
Often return to normal once the trigger improves.
Examples of triggers include:
- viral infections
- stress or acute illness
- recent surgery
- steroid medications
Medical treatments
Some therapies lower lymphocytes.
Examples include:
- chemotherapy
- radiation
- immune-suppressing medicines
Chronic medical conditions
Examples include:
- autoimmune conditions
- certain chronic inflammatory conditions (including sarcoidosis)
- some cancers
- kidney or liver disease
- chronic infections, including HIV
Aging
Lymphocyte counts may slowly decline with age and often do not cause problems.
Nutritional causes (uncommon)
Severe nutritional deficiencies can lower lymphocyte levels.
Examples include:
- protein–calorie malnutrition
- severe zinc deficiency
- severe folate or B12 deficiency (usually with other low blood counts)
These are far less common than temporary or treatment-related causes.
Rare bone marrow-related causes
Some rare conditions affect the early cells in the bone marrow that eventually become lymphocytes.
These conditions are uncommon, and most lymphocytopenia is not caused by bone marrow disease.
Examples include:
- disorders that reduce early lymphoid cell production
- bone marrow infiltration (e.g., cancer, granulomas)
- severe aplastic anemia or marrow failure
- certain chemotherapy effects on early marrow cells
Inherited or genetic causes
Certain rare inherited conditions can affect how the immune system develops or functions and may lead to low lymphocyte counts. These are uncommon, usually start in childhood, and are not the cause in the vast majority of adults with lymphocytopenia.
Examples include:
- immune-system development disorders
- rare genetic conditions that affect lymphocyte survival or function
Your doctor will consider these only if the pattern is unusual or begins early in life.
Does it cause symptoms?
Many people with lymphocytopenia have no symptoms, especially when the count is only mildly low.
When symptoms occur, they usually reflect infection, such as:
- fever or chills
- cough or trouble breathing
- sore throat
- skin infections
- pain with urination
Is it dangerous?
Most cases are not dangerous, especially when the count is mildly low.
Lymphocytopenia matters more when:
- lymphocyte counts are very low
- you are receiving chemotherapy
- you take immune-suppressing medications
- you have a chronic illness that weakens immunity
Very low lymphocyte counts make infections harder to fight.
How your doctor evaluates it
- repeat CBC, to confirm the finding and assess trends
- blood smear, to evaluate cell appearance
- viral testing, such as HIV when clinically appropriate
- medication review, as some medicines lower lymphocytes
- autoimmune or inflammatory testing, if symptoms suggest autoimmune disease
- nutritional assessment, to check for deficiencies
- bone marrow testing, reserved for very low counts, multiple abnormal blood counts, or concern for marrow disease
Not everyone needs all of these tests.
How it is treated
In many people, no treatment is needed.
Treatment depends on the cause:
- temporary lymphocytopenia → often no treatment
- medication-related → adjusting medicines may help
- infection-related → treatment may raise the count
- nutritional deficiency → replacement if needed
- chronic or severe lymphocytopenia → closer monitoring
Many people only need periodic follow-up CBCs.
Daily life and self-care
- follow your doctor’s advice about medications and treatments
- wash your hands often
- avoid close contact with people who are sick
- report symptoms of infection early
- maintain good sleep, nutrition, and activity
When should I contact my doctor?
Contact your doctor if you have:
- fever or chills
- cough or trouble breathing
- pain with urination
- redness, swelling, or worsening skin changes
- frequent or lingering infections
Seek urgent care for:
- high fever
- confusion
- difficulty breathing
What is the usual plan going forward?
Your doctor will:
- monitor your lymphocyte count over time
- repeat the CBC if symptoms develop or if counts change
- track any trends to see whether the count is stable, rising, or falling
- decide whether additional testing is ever needed
Most people see their lymphocyte count return to normal or stay mildly low and stable without causing problems.
Long-term follow-up is usually simple and infrequent.
Making sense of it
Think of lymphocytes as a team of detectives who patrol your body looking for trouble. On some days, more of them are out in the tissues following leads, and fewer are passing through the bloodstream when we “take attendance.” A low count on a blood test may simply mean the detectives were busy elsewhere, not that the team is missing.
A low lymphocyte count is common and often temporary, especially after minor illnesses, stress, or recent infections. In most otherwise healthy people, it does not mean weaker immunity, and the count often returns to normal on its own unless there is an underlying condition.
Your doctor’s job is to make sure this pattern fits a safe explanation for you.
Key takeaways
- most lymphocytopenia is mild or temporary and often improves on its own
- a single low value is common and does not always mean weak immunity
- infection risk increases mainly when counts are very low or during specific treatments
- good hygiene and early attention to symptoms help keep you safe
- your doctor will guide follow-up and most people do very well with simple monitoring
For clinicians: Read our detailed guide on how to communicate about lymphocytopenia to patients.
