For Your Healthcare Provider
Have your patient scan this QR code with their smartphone camera to instantly access this educational guide on their device.

A guide for patients with anemia caused by iron deficiency
Access the Resources
Note: The video and audio linked above were generated with the assistance of AI. Clinical accuracy has been reviewed, but no AI-generated content can be guaranteed to be fully error-free.
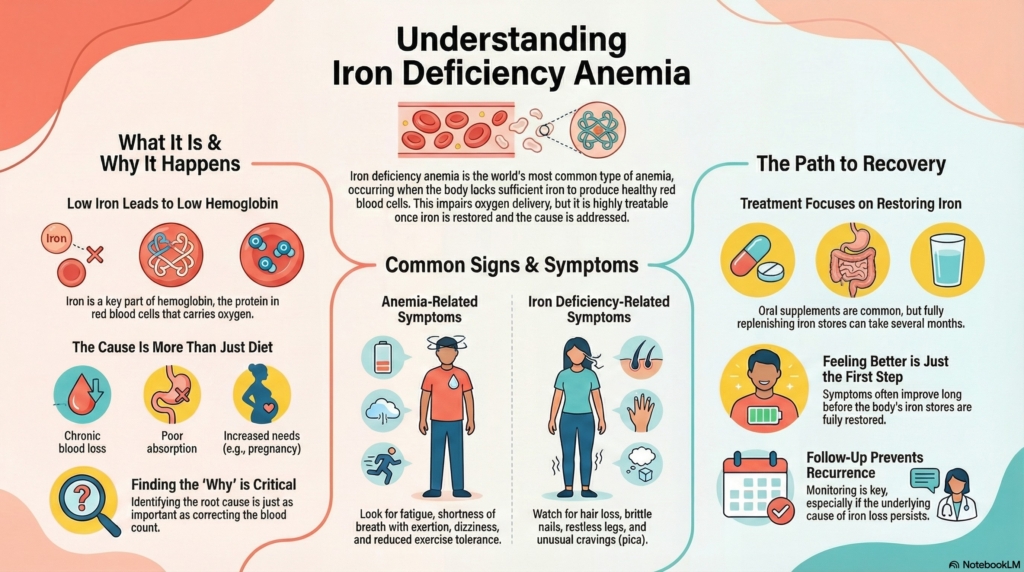
Iron deficiency anemia is a common condition in which the body does not have enough iron to make healthy red blood cells.
It is often treatable, and most people improve once iron stores are restored and the underlying cause is addressed.
First things first
Iron deficiency anemia means that the hemoglobin level is low because the body does not have enough iron to produce red blood cells normally.
This is the most common type of anemia worldwide. It often develops gradually, and symptoms may be subtle at first, which is why it is frequently discovered on routine blood testing.
Early care focuses on two questions: whether anemia is present and why iron levels are low. Treatment addresses both restoring iron and identifying the cause.
What it is
Iron deficiency anemia occurs when iron stores become depleted to the point that red blood cell production is impaired.
Iron is an essential building block for hemoglobin, the protein inside red blood cells that carries oxygen. When iron stores become too low, the body cannot make enough hemoglobin, so red blood cells carry less oxygen. Over time, this leads to anemia.
This condition exists on a spectrum. Some people first develop iron deficiency without anemia, followed by iron deficiency anemia if iron losses continue or intake or absorption are inadequate.
Why it happens (causes)
Iron deficiency anemia develops when iron losses or requirements exceed intake or absorption over time.
Common contributors include:
- chronic blood loss, such as menstrual bleeding or bleeding from the gastrointestinal tract
- reduced dietary iron intake, most often in people who avoid meat
- impaired absorption from the gut, including conditions such as celiac disease, prior bariatric surgery, chronic acid suppression, or certain infections
- increased iron needs during pregnancy, growth, or periods of endurance exercise
- recurrent blood donation
In adults who do not menstruate, blood loss from the stomach or intestines is an especially important cause to evaluate. In menstruating individuals, gastrointestinal evaluation is usually guided by age, symptoms, and clinical judgment.
Does it cause symptoms?
Yes, often.
Symptoms of iron deficiency anemia reflect both anemia itself and low iron stores. Some people notice mild fatigue, while others experience symptoms that interfere with daily activities.
Symptoms related to anemia may include fatigue, shortness of breath with exertion, reduced exercise tolerance, dizziness, or headaches.
Symptoms related to iron deficiency may include low energy, difficulty concentrating, hair thinning or hair loss, brittle or ridged nails, changes in nail shape, cold intolerance, pica, restless legs, or tinnitus.
How a person feels often depends on how low the hemoglobin level is and how quickly it declined.
Is it dangerous?
For most people, iron deficiency anemia is not immediately dangerous, but it should not be ignored.
If anemia is severe or long-standing, it can strain the heart, worsen existing medical conditions, and significantly affect quality of life. During pregnancy, untreated iron deficiency anemia can increase risks for both the mother and baby.
Just as important, iron deficiency anemia can signal ongoing blood loss or poor absorption. Identifying and addressing the cause matters, not just correcting the blood count.
How your doctor evaluates it
Evaluation begins by confirming anemia and iron deficiency with blood tests.
Doctors commonly review:
- hemoglobin and red blood cell indices
- ferritin to assess iron stores
- iron levels and transferrin saturation
- trends over time rather than a single result
Once iron deficiency anemia is confirmed, the next step is identifying the cause. This may involve gynecologic evaluation, gastrointestinal testing, dietary review, or assessment for absorption problems, depending on age, sex, symptoms, and risk factors.
What is the treatment?
Treatment focuses on restoring iron stores and addressing the underlying cause.
Many people are treated with oral iron supplements, which are effective but require time and consistent use. Hemoglobin levels often begin to rise within a few weeks, but full repletion of iron stores usually takes several months.
Some people are advised to take iron once daily or every other day to improve absorption and reduce side effects. Taking more iron than recommended does not speed recovery and can interfere with absorption.
In some situations, such as poor absorption, intolerance to oral iron, ongoing blood loss, or the need for faster correction, intravenous iron may be recommended.
Daily life and self-care
Dietary iron can support recovery, but diet alone is rarely enough to correct iron deficiency anemia once anemia is present. Most people need iron supplementation and time for the body to rebuild healthy red blood cells.
Taking iron as prescribed, avoiding unnecessary interruptions, and understanding that recovery is gradual can reduce frustration. Many people begin to notice symptom improvement within weeks, while full restoration of iron stores often takes several months, even after hemoglobin improves.
Addressing contributing factors, such as heavy menstrual bleeding, digestive symptoms, or recurrent blood loss, is an essential part of long-term care, not just short-term treatment.
Helpful self-care strategies may include:
- taking iron exactly as directed, even after you start to feel better
- being patient with gradual improvement in energy and stamina
- keeping follow-up appointments and blood tests to confirm recovery
- working with your care team to address contributors, such as heavy periods or gastrointestinal symptoms
When should I contact my doctor?
You should contact your doctor if symptoms persist or worsen despite treatment, or if new symptoms develop.
Follow-up is especially important if hemoglobin or iron levels do not improve as expected, if anemia returns after treatment, or if side effects make iron therapy difficult to continue. Staying in touch helps ensure that treatment is working and that the underlying cause has been adequately addressed.
Reach out to your clinician if:
- fatigue, shortness of breath, or other symptoms do not improve after starting treatment
- blood counts or iron levels remain low or fall again after therapy
- side effects make it hard to continue iron treatment
- new symptoms appear that concern you
Seek urgent medical care if you develop chest pain, shortness of breath at rest, severe dizziness, or feel like you might faint.
What is the usual plan going forward?
Most clinicians monitor hemoglobin and iron studies over time to confirm improvement.
Once anemia resolves and iron stores are replenished, treatment may be stopped or continued at a lower maintenance dose depending on the cause. If the underlying cause persists, iron deficiency can recur over time, and follow-up testing helps detect this early.
Plans are individualized and may change as medical conditions, bleeding patterns, or life circumstances evolve.
Making sense of it
Iron deficiency anemia reflects both a shortage of iron and the body’s response to that shortage.
Understanding that anemia is a consequence, not the root problem, explains why care focuses on restoring iron and identifying the cause. With appropriate treatment and follow-up, most people recover well and regain normal energy and function.
Key takeaways
- iron deficiency anemia is common and treatable, and most people recover with appropriate care
- low iron leads to low hemoglobin, which reduces oxygen delivery in the body
- symptoms may reflect anemia, iron deficiency, or both, and severity varies
- treatment restores iron but takes time, even after symptoms improve
- finding and addressing the cause matters, because it helps prevent recurrence
If you’d like to go deeper:
Our guide to living with iron deficiency covers diet, supplements, recurrence, and day-to-day questions that often come up after diagnosis or treatment.
If treatment is needed, our overview of oral versus IV iron therapy explains how these options differ in speed, convenience, and side effects.
For clinicians: Read our detailed guide on how to communicate about iron deficiency anemia to patients.
