For Your Healthcare Provider
Have your patient scan this QR code with their smartphone camera to instantly access this educational guide on their device.

A guide for patients with elevated immature granulocytes
Access the Resources
Note: The video and audio linked above were generated with the assistance of AI. Clinical accuracy has been reviewed, but no AI-generated content can be guaranteed to be fully error-free.
Immature granulocytes (IG) are young white blood cells that usually stay in the bone marrow. A small number can appear in the bloodstream during infection, inflammation, or physical stress, and this is most often temporary and not dangerous.
First things first
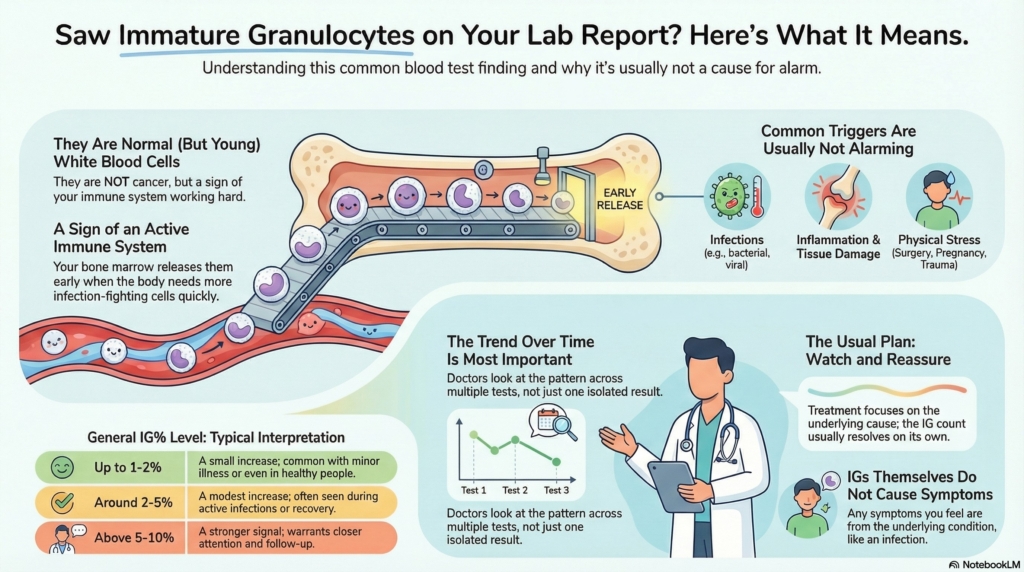
Immature granulocytes are not cancer cells. They are normal white blood cells that have entered the bloodstream a little earlier than usual.
Modern blood analyzers are more sensitive than older methods, so many people now see a small nonzero IG value on routine labs that might have been reported as “0” in the past.
Most cases are mild and reflect bone marrow activity, not a bone marrow disease.
What are granulocytes?
Granulocytes are a group of white blood cells that help the body respond to infection and inflammation. They include:
- neutrophils (the most common type)
- eosinophils
- basophils
Granulocytes are made in the bone marrow and released into the bloodstream when they are mature and ready to work.
What are immature granulocytes?
Immature granulocytes are early forms of granulocytes that are usually kept inside the bone marrow while they finish developing.
When the body needs more infection-fighting cells quickly, the marrow may release some cells slightly early into the bloodstream. Think of this as the immune system responding quickly, not malfunctioning.
Most of what laboratories group as “immature granulocytes” are late-stage cells that are close to mature. Earlier forms are less common and may prompt closer follow-up if they persist.
How immature granulocytes are measured
Immature granulocytes are measured automatically as part of a complete blood count (CBC) with differential.
They may be reported as:
- a percentage (IG%), and/or
- an absolute immature granulocyte count
The lab may also comment on the presence of specific immature forms on a blood smear when that is checked.
Ranges that matter
In healthy people, immature granulocytes are usually absent or present at very low levels.
Small increases are common, especially during everyday illnesses. As a general guide (exact cutoffs vary by lab and clinical setting):
- very small increases (for example, an IG% up to about 1–2%) can be seen during common infections, inflammation, or even in otherwise healthy people
- modest increases (for example, around 2–5%) are often seen during infections, recovery from illness, or physiologic stress
- higher levels (for example, above about 5–10%) usually reflect a stronger inflammatory or infectious signal and warrant closer attention to the overall picture and follow-up testing
Your doctor focuses on the trend over time, your symptoms, the total white blood cell count, and the rest of the differential, not a single IG result.
Immature granulocytes can also be seen more commonly in certain normal physiologic situations, such as pregnancy, and in newborns and children fighting infections.
Why immature granulocytes appear
Common reasons include:
- infections (especially during active infection or early recovery)
- inflammation
- physical stress (such as surgery, trauma, or severe illness)
- recovery after bone marrow suppression
- medications that affect white blood cell production (for example corticosteroids or growth factors)
Very rarely, persistent or rising IG levels without a clear explanation, especially when paired with other abnormal blood tests or systemic symptoms, may prompt evaluation for less common bone marrow problems.
Does it cause symptoms?
Immature granulocytes themselves do not cause symptoms.
If symptoms are present, they usually come from the underlying condition causing the IG value to rise (for example, infection or inflammation), not from the immature cells in the blood.
Many people discover this finding only because it appears on routine blood work.
Is it dangerous?
In most cases, no.
A mild or temporary increase in immature granulocytes is often part of a normal immune response. Concern increases when:
- the IG level is persistent or rising
- the total white blood cell count is very high or very low
- other blood counts (hemoglobin or platelets) are abnormal
- the differential shows unexpected abnormalities
- symptoms suggest more than a routine infection or inflammatory flare
Very high white blood cell counts combined with many immature cells may require additional testing to distinguish a strong infection response from a blood disorder. This is uncommon and usually evident from the overall pattern.
How your doctor evaluates it
Evaluation is guided by the overall clinical picture, not a single number.
Your doctor may:
- review symptoms and recent illnesses
- review medications and recent medical events
- look at the total white blood cell count and balance of cell types
- compare with prior blood tests to assess trends
- repeat the CBC after time has passed
If abnormalities persist or the pattern is concerning, additional tests or referral to a blood specialist may be recommended.
How is it treated
There is no treatment aimed at immature granulocytes themselves.
Management focuses on:
- treating the underlying cause, if one is identified
- monitoring blood counts until they return toward baseline
In many cases, the IG value settles on its own.
Daily life and self-care
In most cases, no special self-care is needed for immature granulocytes.
There are usually no diet or activity restrictions. The most helpful steps are:
- following treatment plans for any underlying condition
- taking medications only as directed
- keeping follow-up appointments for repeat testing
When should I contact my doctor?
Contact your doctor if you develop new or worsening symptoms, including:
- persistent fever or worsening signs of infection
- unexplained night sweats or weight loss
- easy bruising or bleeding
- new or worsening symptoms
- repeat blood tests showing rising or persistent abnormalities
If you feel well and follow-up has been recommended, it is reasonable to wait for the planned recheck.
What is the usual plan going forward?
For most people, the plan is observation and reassurance.
This often includes:
- repeating the CBC after a short interval
- watching the trend rather than reacting to a single result
- treating any underlying condition if present
Only a small minority of patients need extensive testing or long-term follow-up.
Making sense of it
Immature granulocytes are best thought of as a marker of bone marrow activity, not a diagnosis.
They are like backup responders released when the body wants to be prepared. Most of the time, the count returns toward normal as the underlying trigger resolves.
Key takeaways
- IG reflects marrow activity, not cancer
- small increases are common with infection or stress
- IG does not cause symptoms
- patterns over time matter more than one value
- persistent elevation with other abnormalities may need closer evaluation
For clinicians: Read our detailed guide on how to communicate about IGs to patients.
