Treatment

The patient had worsening mental status in the Emergency Department. She was intubated for airway protection and admitted to the medical intensive care unit. She did not require pressor support. Her urine output, urea and creatinine improved with fluids.
What are treatment options for her hematological status when first admitted?
Let’s return to the concept of critical oxygen delivery. Recall the plot of oxygen delivery against oxygen consumption. Our patient, even with the most efficient of cardiovascular adaptations, will be squarely on the supply-dependent part of the curve. This means that any further reduction in oxygen delivery will lead to anaerobic metabolism and increased lactic acid production.
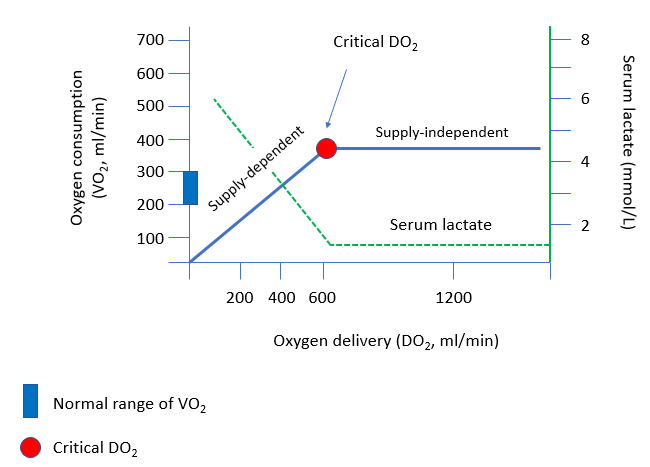
The surest way to offset this risk is to transfuse the patient. However, some patients, such as Jehovah Witnesses, do not accept blood transfusions. How would you manage a case such as this without transfusion support (see next slide for answer)?
There are several possible non-transfusion interventions:
- Use sedation and/or neuromuscular block to minimize oxygen demand.
- Administer hematinic agents, for example IV iron in a case of iron deficiency.
- Administer erythropoietin.
- Deliver high oxygen concentration or use hyperbaric oxygen therapy to increase the level of plasma-dissolved oxygen.
- Investigational therapeutics such as artificial oxygen carriers.
Additional history from the patient’s family confirmed that the patient had experienced years long history of chronic abnormal uterine bleeding. A CTAP showed massively enlarged uterus measuring 17.8 x 12.0 x 15.4 cm, which was hyperenhancing and concerning for malignancy:

She ultimately had a EXPLORATORY LAPAROTOMY, TOTAL ABOMINAL HYSTERECTOMY, BILATERAL SALPINGO-OOPHORECTOMY, LYMPH NODE BIOPSY, which showed the following:

Thus, the diagnosis was fibroids.
