Treatment

How would you treat this patient?
How would you treat this patient with thrombotic thrombocytopenic purpura (TTP)?
Overview of treatment of thrombotic thrombocytopenic purpura (TTP):
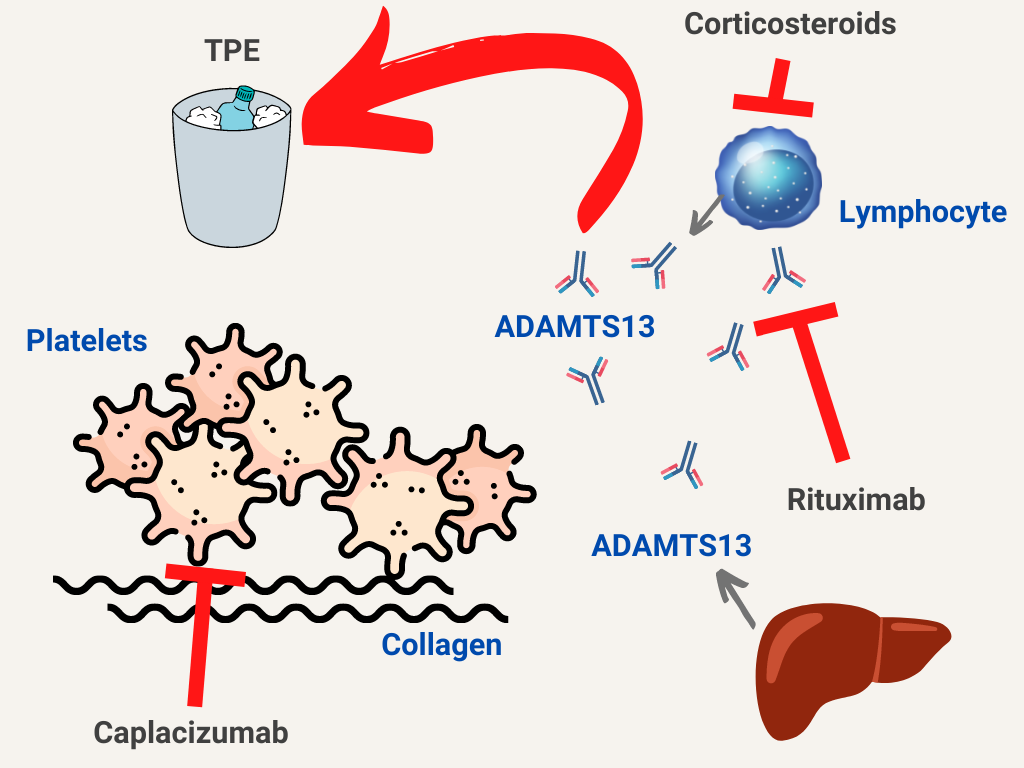
Pathophysiological basis for treatment:
- von Willebrand factor (vWF) normally promotes interactions between platelets and the blood vessel wall.
- vWF circulates as multimers of varying size; the largest of these multimers (called ultra-large multimers) are the most functionally (hemostatically) active.
- Normally, the protease ADAMTS13, which is synthesized by the liver, cleaves circulating ultra-large vWF multimers, preventing excessive platelet-vessel wall interactions.
- Immune TTP is caused by antibody-mediated reduction in ADAMTS13 levels.
- ADAMTS13 deficiency results in excessive ultra-large vWF multimers, leading to uncontrolled platelet activation, adhesion and aggregation, microvascular thrombosis and tissue ischemia.
Treatment approaches:
- Remove antibodies against ADAMTS13 – therapeutic plasma exchange (TPE) – the mainstay of treatment
- Replenish ADAMTS13 – TPE
- Block von Willebrand factor-platelet interactions – caplacizumab
- Inhibit production of antibodies against ADAMTS 13 – corticosteroids, rituximab
How rapdily should plasma exchange be initiated?
How rapidly should plasma exchange be initiated?
What blood test should be sent off before plasma exchange begins?
What blood test should be sent off before plasma exchange begins?
How does plasma exchange work in thrombotic thrombocytopenia purpura (TTP)?
How does plasma exchange work in thrombotic thrombocytopenia purpura (TTP)?
Plasma exchange (together with corticosteroids) is the standard initial therapy for patients with thrombotic thrombocytopenia purpura (TTP):
- Plasma exchange should not be delayed while waiting for confirmatory ADAMTS13 measurement, especially if the patient has a high clinical suspicion of TTP.
- Since ADAMTS13 activity level is usually a send-out out test, plasma exchange is typically initiated before ADMATS13 levels are available.
- Plasma exchange is typically continued until platelet count > 150 × 109/L and lactate dehydrogenase is near normal for 2-3 consecutive days.
For additional information about TPE in TTP, click here.
Other treatment options (which may be added to therapeutic plasma exchange and corticosteroids) include:
- Rituximab:
- Antibody that targets CD20 antigen present on B lymphocytes.
- Inhibits B cell production of anti-ADAMTS13 antibodies, which are present in patients with immune ITP.
- While often reserved for refractory or relapsing TTP, may be used up front with plasma exchange and corticosteroids in newly diagnosed TTP.
- Dose: 375 mg/m2 IV weekly for 4 weeks.
- For additional information about rituximab in TTP, click here.
- Caplacizumab:
- Humanized anti-von Willebrand factor (vWF) single-variable-domain immunoglobulin (nanobody) that targets AI domain of vWF, preventing its interaction with platelet glycoprotein 1b-IX-V.
- FDA approved for treatment of adults with immune TTP in combination with plasma exchange and immunosuppressive therapy.
- Does not correct underlying ADAMTS13 deficiency nor does it eliminate anti-ADAMTS13 autoantibodies.
- Must be given with immunosuppressive treatments such as rituximab and corticosteroids.
- On day 1, administered IV and SQ on day 1, before and after plasma exchange, respectively; then SQ on subsequent days.
- For additional information about caplacizumab in TTP, click here.
- Transfusions – Platelet transfusions should not be routinely administered, but may be given in cases of severe or life-threatening hemorrhage. Platelet transfusions have been shown to be associated with higher odds of arterial thrombosis and mortality among patients with TTP. Learn more here.
- Thromboprophylaxis with low-molecular-weight heparin (LMWH) once the platelet count has reached > 50 × 109/L in patients with active hemolysis.
- Folate supplementation
Overview of treatment pre- and post-ADAMTS13 levels:
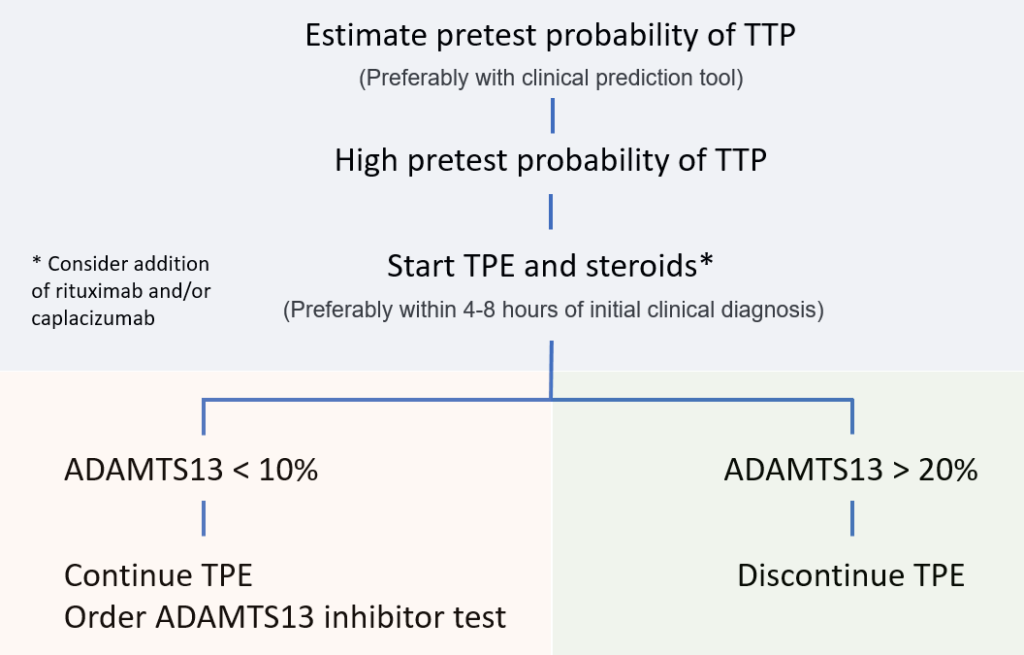
Our 56 year-old patient received received plasma exchange and corticosteroids on the eve of admission. His mental status normalized within 24 hours of treatment and his platelet counts increased over the ensuing days. His ADAMTS13 level returned at <10%, consistent with a diagnosis of thrombotic thrombocytopenic purpura (TTP). Plasma exchange was continued until his platelet count was > 150 x 109/L for 3 consecutive days, 9 days following admission. He was discharged home, and followed by a hematologist without evidence of relapse over the next year.
