A brief guide for patients with hemolytic anemia
View on a Mobile Device
Scan to view this guide on your phone.

Access the Resources
Note: The video and audio linked above were generated with the assistance of AI. Clinical accuracy has been reviewed, but no AI-generated content can be guaranteed to be fully error-free.
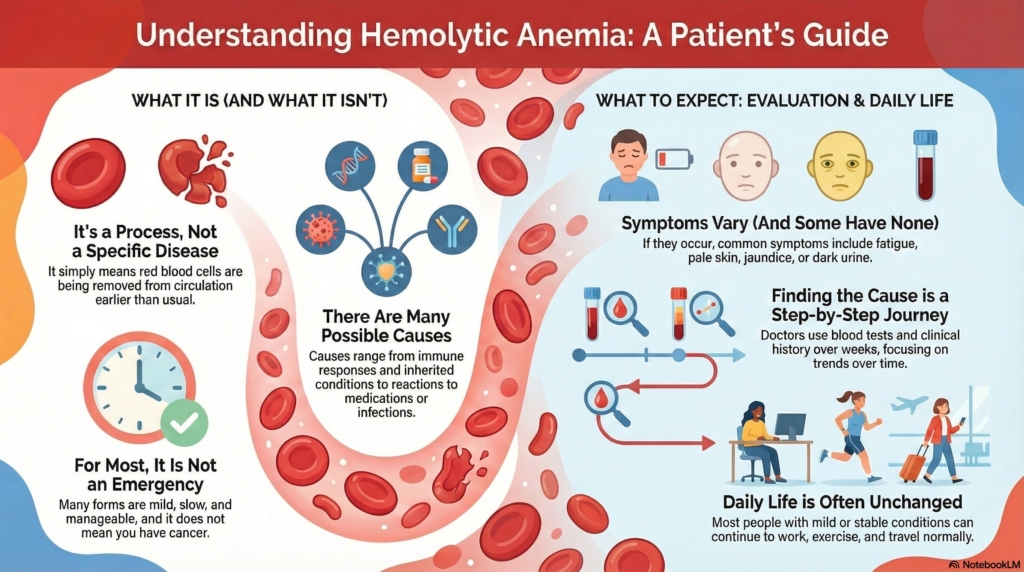
Hemolytic anemia describes what is happening, not why it is happening.
It means red blood cells are being broken down faster than usual, and the body may not be able to replace them quickly enough.
For many people, this process is mild, slow, and manageable, but some people can have a faster or more severe episode at the beginning.
Finding the cause guides next steps, and the workup is usually done over weeks (sometimes a few months), not hours.
First things first
Seeing the words “hemolytic anemia” on a lab report or note can be unsettling.
Many people immediately wonder:
- does this mean cancer or leukemia?
- is my body attacking itself?
- is this dangerous?
- what happens next?
For most patients, hemolytic anemia is not immediately dangerous, and it does not mean cancer.
It is a pattern doctors recognize, and it helps them decide what to look for next.
What it is
Hemolytic anemia means that red blood cells are being removed from circulation earlier than usual.
Normally, red blood cells circulate for about 120 days.
In hemolytic anemia, some red blood cells are cleared sooner, which can lead to anemia if the bone marrow cannot keep up.
Importantly:
- hemolytic anemia is not a single disease
- it can happen for many different reasons
- the pace can be slow or fast, depending on the cause
Some people have hemolysis with a normal hemoglobin level (the bone marrow is keeping up). Others develop anemia if hemolysis outpaces replacement.
Why it happens (causes)
Doctors broadly think about causes in categories, rather than all at once. They typically start by looking for the most common and treatable causes first.
Common categories include:
- immune-related causes (antibodies shorten the lifespan of red blood cells)
- inherited red blood cell conditions (for example, conditions affecting hemoglobin, the red cell membrane, or red cell enzymes)
- reactions to medications or infections
- mechanical or physical stress on red blood cells (for example, certain artificial heart valves or rare blood vessel abnormalities)
- rare blood or bone marrow disorders
Many patients are told they have evidence of hemolysis before the exact cause is known.
That is a normal and expected step in the evaluation.
Does it cause symptoms?
Some people have no symptoms at all, and hemolysis is found only on blood tests.
When symptoms occur, they may include:
- fatigue or low energy
- shortness of breath with exertion
- pale skin
- yellowing of the eyes or skin (jaundice)
- dark urine (tea-colored or cola-colored)
- lightheadedness or feeling faint
Symptoms depend mainly on how fast hemolysis is happening and whether anemia develops.
Is it dangerous?
For most people, hemolytic anemia is not an emergency.
Key points:
- many forms are mild and stable once the cause is understood
- serious complications are uncommon without clear warning signs
- doctors monitor trends, not single lab values
- treatment decisions are based on symptoms and severity, not the word “hemolysis” alone
Life expectancy is normal for most people with hemolytic anemia. In a smaller number of patients, long-term outlook depends on the underlying cause, which is why identifying the cause matters.
How your doctor evaluates it
Evaluation usually includes a combination of blood tests and clinical history.
Doctors often look at:
- hemoglobin level
- reticulocyte count (new red blood cells)
- bilirubin
- LDH
- haptoglobin
- direct antiglobulin test (also called a Coombs test)
- blood smear (a look at the blood under a microscope)
These tests help confirm hemolysis and point toward the most likely category of cause.
What does “immune” vs “non-immune” hemolysis mean?
This distinction helps guide next steps.
Immune hemolysis means antibodies are involved in red blood cell breakdown.
Non-immune hemolysis means red blood cells are being broken down for other reasons.
This does not automatically mean an autoimmune disease, cancer, or a lifelong condition. Some immune causes are temporary (for example, related to an infection or a medication), and many non-immune causes are manageable once identified.
What is the treatment?
Treatment depends on the cause, the severity, and whether symptoms are present.
Many patients:
- do not need immediate treatment
- are monitored over time while the cause is clarified
- need treatment only if anemia worsens or symptoms develop
Examples of treatment (depending on the cause) may include:
- stopping a triggering medication
- treating an underlying infection
- medicines that reduce immune-driven hemolysis
- treatments specific to inherited conditions
- blood transfusion if anemia is severe or symptoms are significant
When transfusions are needed, they are usually used to stabilize symptoms while the underlying cause is addressed.
Daily life and self-care
Most people with mild or stable hemolytic anemia:
- work and exercise normally
- travel without restrictions
- live full, active lives
Helpful steps include:
- keeping follow-up appointments while the cause is being clarified
- reporting new or worsening symptoms
- letting clinicians know before surgery or major illness
- avoiding unnecessary worry over a single lab result
If you feel well and your hemoglobin is stable, it is usually safe to continue normal routines.
When should I contact my doctor?
You should contact your care team if you notice:
- increasing fatigue, shortness of breath, or reduced exercise tolerance
- yellowing of the eyes or skin
- dark urine that is new or worsening
- new or worsening symptoms, or a rapid change from your usual baseline
- questions about medications, infections, or upcoming procedures
These situations usually lead to planning and adjustment, not emergency care.
Seek urgent care right away if you have:
- chest pain, severe shortness of breath, fainting, or confusion
- rapidly worsening weakness
- severe symptoms plus a known very low hemoglobin level
What is the usual plan going forward?
For most patients, the plan includes:
- confirming that hemolysis is present and tracking trends
- identifying the cause (often in a stepwise way)
- monitoring blood counts and markers over time
- treating only if necessary
- adjusting care if symptoms change
Many people are followed over time with little disruption to daily life once a stable pattern is established.
Making sense of it
Hemolytic anemia is best thought of as a process, not a diagnosis.
It tells doctors how red blood cells are behaving, not why.
Once the cause is clarified, care becomes more focused and predictable.
Key takeaways
- process, not a diagnosis: hemolytic anemia describes red blood cells breaking down early, not a single disease
- often manageable: many forms are mild, slow, and treatable
- rarely an emergency: serious cases are recognized by symptoms and rapid changes, and treated promptly
- stepwise workup: evaluation often takes weeks and focuses on patterns, not one test
- treatment depends on cause: many people need only monitoring, while others need targeted therapy
For clinicians: Read our detailed guide on how to communicate about hemolytic anemia to patients.
