For Your Healthcare Provider
Have your patient scan this QR code with their smartphone camera to instantly access this educational guide on their device.

A guide for patients with anemia associated with inflammation
Access the Resources
Note: The video and audio linked above were generated with the assistance of AI. Clinical accuracy has been reviewed, but no AI-generated content can be guaranteed to be fully error-free.
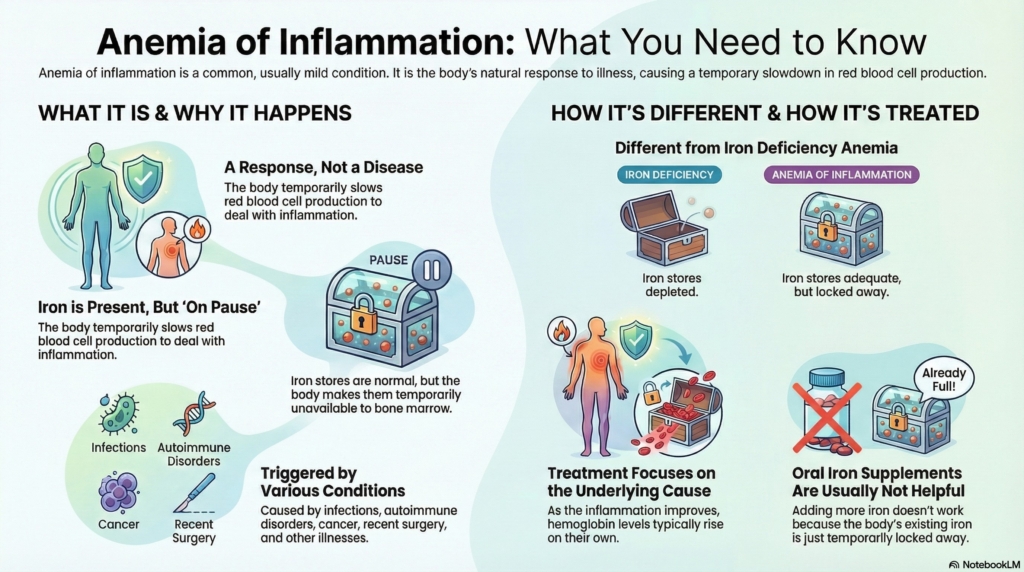
Anemia of inflammation is a common type of anemia that occurs when the body is responding to illness or inflammation.
It is not a disease of the blood itself and is usually mild, stable, and improves as the underlying condition improves.
First things first
Anemia of inflammation is one of the most common reasons people have a low hemoglobin level.
This condition used to be called anemia of chronic disease, but that name is misleading. It does not need to be chronic, it can develop relatively quickly, and it is not a disease by itself. Instead, it reflects how the body responds when there is inflammation somewhere else in the body.
Understanding this distinction helps explain why this type of anemia is often not dangerous and why treatment focuses on the underlying condition rather than the blood count alone.
What it is
Anemia of inflammation occurs when the body temporarily slows red blood cell production during inflammation.
Iron is still present in the body, often in normal or even increased amounts, but it is not available to the bone marrow where red blood cells are made. Because of this, hemoglobin levels fall modestly, leading to anemia.
This pattern is sometimes called functional iron deficiency, meaning iron is present but temporarily inaccessible, rather than truly missing.
Why it happens (causes)
Inflammation changes how the body handles iron and red blood cell production.
During illness or inflammatory states, the body shifts priorities. Iron is held back from circulation, and red blood cell production slows. This is a coordinated response rather than a failure of the bone marrow.
Inflammation can come from many sources, not just infection. Autoimmune conditions, cancer, chronic medical illnesses, inflammatory bowel disease, recent surgery or trauma, and other inflammatory states can all trigger this response.
How this differs from iron deficiency anemia
Anemia of inflammation is different from iron deficiency anemia.
In iron deficiency anemia, iron stores are depleted and iron replacement is essential. In anemia of inflammation, iron stores are usually adequate, but iron is temporarily unavailable.
Because of this difference, treatments that work well for iron deficiency anemia, such as oral iron supplements, are often much less effective in anemia of inflammation.
In some people, both conditions can occur together. When this happens, doctors interpret iron studies carefully and may recommend iron treatment if true iron deficiency is also present.
Does it cause symptoms?
Sometimes.
Symptoms depend on how low the hemoglobin level is and how quickly it changed. Many people have few or no symptoms, while others may notice fatigue, reduced stamina, or shortness of breath with exertion.
How a person feels often reflects the underlying illness or inflammation as much as the anemia itself.
Is it dangerous?
For most people, anemia of inflammation is not dangerous.
It is usually mild to moderate and tends to level off rather than continue to worsen.
Severe drops in hemoglobin are uncommon unless another condition is present.
If anemia becomes severe or progresses quickly, doctors look for additional causes such as bleeding, true iron deficiency, kidney disease, medication effects, or other blood disorders.
How your doctor evaluates it
Doctors recognize anemia of inflammation by looking at patterns rather than a single lab value.
Blood tests often show a low hemoglobin level with iron studies that appear confusing at first glance. Ferritin may be normal or high, while circulating iron levels may be low. Markers of inflammation are often elevated.
The overall clinical context, including medical history, inflammatory markers, and trends over time, is key to making the diagnosis and distinguishing this condition from other causes of anemia.
What is the treatment?
Treatment focuses on addressing the underlying inflammatory condition.
As inflammation improves, hemoglobin levels often rise on their own over weeks to months.
Oral iron supplements are usually not helpful, because iron is already present but temporarily unavailable.
Intravenous iron is not routinely used and may be avoided during active infection.
In selected situations, such as certain kidney or cancer-related conditions, medications that stimulate red blood cell production may be considered, but these are not standard treatments for uncomplicated anemia of inflammation.
Daily life and self-care
Most people do not need to change daily activities because of anemia of inflammation.
Managing the underlying condition and keeping follow-up appointments are the most important steps.
Energy levels often improve gradually as inflammation settles. Trying to increase iron intake on your own, through supplements or diet, is usually not helpful and may add side effects without benefit unless your clinician specifically recommends it.
When should I contact my doctor?
You should contact your doctor if symptoms worsen, if new symptoms develop, or if anemia does not improve over time.
Follow-up is especially important if hemoglobin levels fall further or if symptoms such as shortness of breath, chest discomfort, or dizziness appear.
Seek urgent medical care if you develop chest pain, severe shortness of breath at rest, or feel like you might faint.
What is the usual plan going forward?
Doctors usually monitor hemoglobin levels and markers of inflammation over time.
The goal is to confirm that the anemia remains stable, symptoms are manageable, and the underlying condition is being treated effectively. Mild anemia may persist while inflammation is active and often improves gradually as inflammation settles.
If hemoglobin levels fall further, symptoms worsen, or inflammation improves without improvement in anemia, doctors reassess for additional contributors such as iron deficiency, bleeding, kidney disease, or medication effects.
Making sense of it
It can help to think of anemia of inflammation as iron being temporarily on pause.
The body is protecting and redistributing resources while dealing with inflammation. As that process resolves, iron becomes available again and red blood cell production recovers.
Key takeaways
- common and usually mild: anemia of inflammation is frequently seen and rarely severe
- not a blood disease: it reflects a response to inflammation elsewhere in the body
- iron is present: iron stores exist but are temporarily unavailable for red blood cell production
- treat the cause: managing the underlying condition is the main approach
- often improves over time: hemoglobin levels typically rise as inflammation settles
For clinicians: Read our detailed guide on how to communicate about anemia of inflammation to patients.
