When a disease reorganizes time, memory, and self
Note: The video and audio linked above were generated with the assistance of AI. Clinical accuracy has been reviewed, but no AI-generated content can be guaranteed to be fully error-free.
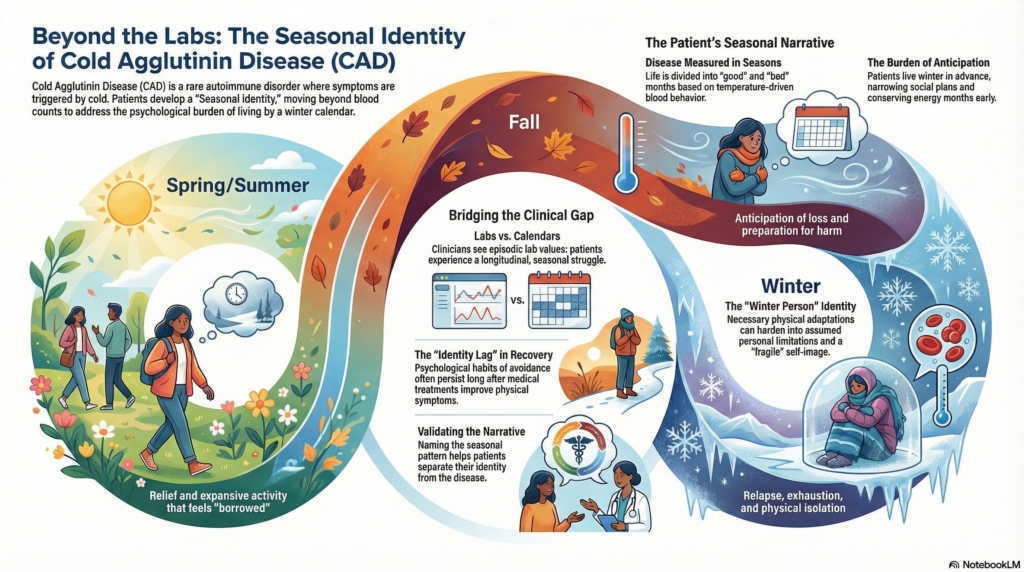
Unlike continuous chronic illnesses, CAD unfolds as a seasonal experience. Symptoms rise and fall with temperature, anticipation precedes winter, and identity can become organized around the cold months. The diagram contrasts laboratory time with lived time, illustrating how patients experience the disease as chapters in a yearly cycle rather than as isolated clinical events.
When a disease reorganizes time, memory, and self
For many patients with cold agglutinin disease, winter is not just a season.
It is a chapter in the patient’s life.
Long before diagnosis, patients often notice a pattern. Symptoms arrive with cold months and recede with warmth. Fatigue deepens. Hands discolor. Pain appears at the margins. Energy contracts inward. Life narrows.
Over time, patients do not simply experience winter differently.
They begin to organize their lives around it.
When illness becomes seasonal
Most chronic diseases are continuous. Cold agglutinin disease is episodic, environmental, and cyclical. Symptoms wax and wane with temperature more than clock time.
For many patients, this creates a distinctive illness narrative:
- summer feels like remission
- winter feels like relapse
- fall brings anticipation, not just of weather, but of loss
- spring carries relief that feels earned
Patients rarely describe this as unpredictability. They describe it as expectation. The disease does not surprise them. It returns on schedule.
Illness, in CAD, is not measured only in years.
It is measured in seasons.
Not every patient experiences this pattern cleanly. Some have more year-round burden, while others in warmer climates feel the cycle less sharply. Climate, housing, work, intercurrent illness, and treatment all modify the pattern. Yet the seasonal frame is common enough to shape how many patients understand their disease, and themselves.
Anticipation as a form of burden
One of the least visible burdens of CAD is anticipation.
Patients often begin preparing for winter weeks or months in advance. Clothing choices change. Travel is reconsidered. Social plans narrow. Energy is conserved.
This is not anxiety in the psychiatric sense. It is rational adaptation to predictable harm. But adaptation carries cost.
Winter is not merely endured when it arrives.
It is lived in advance.
The psychological weight of CAD is not only what happens in the cold.
It is knowing that cold is coming.
Becoming a “winter person”
Seasonal illness reshapes identity quietly.
Over time, patients begin to describe themselves in new ways:
“I’m not a winter person.”
“I don’t tolerate cold.”
“I’m fragile in winter, fine in summer.”
These phrases can be simple description. The risk is when description becomes destiny. till, for many patients, extra restriction is rational when the cost of being wrong is high.
What begins as prudent adaptation can harden into assumed limitation. Avoidance becomes personality.
This matters clinically and ethically. Identity shaped by illness can shrink life beyond what disease itself requires.
The boundary between necessary adaptation and unnecessary restriction is rarely obvious, either to patients or clinicians. It is not drawn by fear or strength of will. It is drawn by habit, experience, and uncertainty.
Memory and the uneven calendar
Patients with CAD often remember their lives unevenly.
Winter memories cluster around exhaustion, cancelled plans, physical discomfort, isolation. Summer memories feel expansive, active, almost borrowed from another self.
Life begins to feel divided into “good months” and “bad months,” not by circumstance, but by blood behavior.
In clinic, many patients describe remembering their year through the lens of temperature.
When clinicians see labs, patients feel seasons
Clinicians often practice in laboratory time (visit-to-visit values), while patients live in lived time (season-to-season constraint).
Patients experience it longitudinally and seasonally.
A hemoglobin value may look stable, but the patient is already counting weeks until winter. A reassuring visit in August may feel irrelevant to someone bracing for January.
Temporally attuned care sounds different. It includes questions like:
What happens to you in the cold months, and what do you start changing in advance? What are you most worried about this winter?
Understanding CAD requires attending to time, not just numbers.
Naming winter restores agency
One of the simplest and most powerful clinical interventions in CAD is acknowledgment.
When clinicians name the seasonal nature of the disease, patients often feel immediate relief. Not because symptoms improve, but because experience becomes legitimate.
Saying:
“Many people with CAD experience winter differently.”
“It makes sense that cold months feel harder.”
separates identity from inevitability.
Winter is something that happens to patients.
It is not who they are.
When physiology improves but identity lags
An under-recognized moment comes when treatment works.
Symptoms ease. Fatigue improves. Hemolysis stabilizes. But identity remains seasonal. Patients continue to live as “winter people,” long after winter physiology has softened.
Habits of avoidance persist. Anticipation outlasts need.
This is not simply psychological inertia. It is often cautious wisdom. If the cost of being wrong is high, patients may need more than one winter to trust improvement.
Still, this becomes a different clinical problem from active seasonal disease, and it requires a different response.
Recovery, in CAD, is not only hematologic.
It is narrative.
Helping patients notice the gap between current physiology and inherited habits, gently and without pressure, is part of care.
Reclaiming seasons without denying disease
The goal is not to pretend winter is neutral. It is not.
The goal is to help patients distinguish:
- what must be avoided
- what can be adapted
- what might be reclaimed
Seasonal identity should be descriptive, not deterministic.
Patients with CAD do not need to become winterless people. They need clinicians willing to help them renegotiate winter on humane terms.
What CAD teaches about illness narratives
Cold agglutinin disease reveals something broader about chronic illness.
Disease does not only alter physiology.
It reorganizes calendars, memories, and selves.
By listening to how patients talk about seasons, clinicians gain access to harms that lab values cannot capture, and to recoveries that treatment alone cannot complete.
Key reflections
- CAD is experienced seasonally, not continuously
- anticipation of winter is a real physiologic and psychological burden
- seasonal illness can quietly reshape identity
- naming patterns restores validation and agency
- physiology may improve before identity does
Cold agglutinin disease does not merely respond to winter.
It teaches how illness can take up residence in the calendar itself.
Reflect and Apply
A patient says, “Winter is when my life stops.”
Before adjusting therapy, what questions would help you understand how winter affects their physiology, routines, and identity?
