For Your Healthcare Provider
Have your patient scan this QR code with their smartphone camera to instantly access this educational guide on their device.

A guide for patients with polyclonal hypergammaglobulinemia (a broad increase in antibodies on blood testing)
Access the Resources
Note: The video and audio linked above were generated with the assistance of AI. Clinical accuracy has been reviewed, but no AI-generated content can be guaranteed to be fully error-free.
A high globulin level or a note about an “elevated gamma region” can be confusing when you first see it on a lab report, especially if these terms are unfamiliar.
Globulins are antibodies made by your immune system. When levels are elevated, this usually reflects a normal immune response to common conditions like infection, inflammation, or liver disease, not cancer or bone marrow disease.
Most people have no symptoms, and many elevations improve with time or with treatment of the underlying cause. Your doctor will explain what your results mean and how monitoring keeps you safe.
This guide is for outpatient evaluation of polyclonal hypergammaglobulinemia and does not apply to acute, severe infections, rapidly progressive illness, or inpatient diagnostic emergencies.

First things first
Seeing a high globulin level or a note about an “elevated gamma region” on your report can be unsettling. Most of the time, this finding is not dangerous. Polyclonal hypergammaglobulinemia usually reflects a normal immune response to inflammation, infection, or other common conditions. Many people feel completely well and do not need extensive testing.
What are immunoglobulins?
Immunoglobulins—also called antibodies—are proteins made by plasma cells.
Their job is to help your body fight infections, respond to inflammation, and provide long-term immune memory.
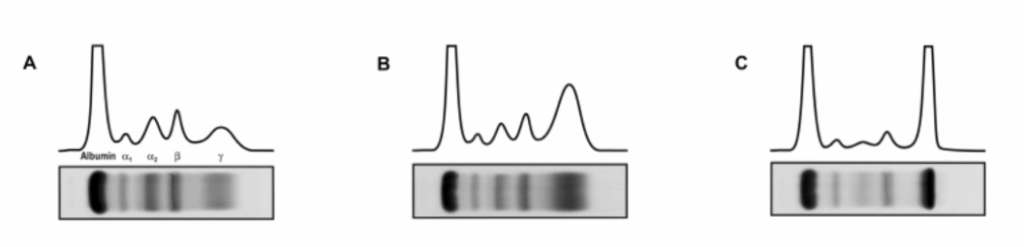
On lab reports, antibody levels appear in the gamma region of tests such as SPEP (serum protein electrophoresis) or as globulin on a standard metabolic panel.
What is polyclonal hypergammaglobulinemia?

Polyclonal hypergammaglobulinemia means that many different immune cells are making many different antibodies, leading to a broad, raised gamma region.
It is not the same as MGUS or a monoclonal spike (“M-spike”).
Most people with polyclonal hypergammaglobulinemia have no symptoms.
It is usually a marker of immune activity rather than a disease on its own.
How antibody levels appear on your lab results
You may see:
- high globulin on a metabolic panel
- elevated gamma region on SPEP
- increased IgG, IgA, or IgM on quantitative immunoglobulin testing
- comments such as “polyclonal increase” or “reactive pattern”
These results indicate immune system activity, not necessarily disease.
Ranges that matter
Normal ranges vary by lab, but common patterns include:
- mild polyclonal elevation (most common)
- moderate elevation (may prompt evaluation for inflammation or liver health)
- marked elevation (may reflect chronic inflammation or long-standing immune activation)
A monoclonal spike is treated differently; your doctor will tell you if this is suspected.
Why antibody levels go up (causes)
Infections (very common)
Your immune system naturally makes more antibodies when fighting infections.
- viral infections
- bacterial infections
- chronic infections (such as hepatitis or HIV)
Inflammation and autoimmune conditions
Chronic inflammation can keep antibody levels mildly elevated.
- rheumatoid arthritis
- lupus
- inflammatory bowel disease
- autoimmune thyroid disease
Liver conditions
Because the liver processes many proteins, liver health influences globulin levels.
- fatty liver
- chronic hepatitis
- cirrhosis
- elevated liver enzymes
Other causes
Rarely, immune or lymphoid disorders
Does it cause symptoms?
Usually no.
Antibody levels themselves do not cause symptoms.
When symptoms occur, they are related to the underlying cause, such as infection or autoimmune activity.
Is it dangerous?
Most cases are not dangerous and do not reflect cancer or bone marrow disease.
Concern increases when:
- other blood counts are abnormal
- a monoclonal pattern is suspected (MGUS or related conditions)
- symptoms such as fevers, night sweats, or weight loss appear
- liver enzymes are significantly abnormal
Your doctor will guide whether further evaluation is needed.
How your doctor evaluates polyclonal hypergammaglobulinemia
CBC
to look for anemia or changes in white cells or platelets
Liver tests
to assess for fatty liver, hepatitis, or other liver conditions
ESR or CRP
to check for inflammation
Hepatitis or autoimmune testing
when suggested by symptoms or history
SPEP and immunoglobulin levels
to confirm that the pattern is polyclonal, not monoclonal
Not everyone needs all tests.
How it is treated
Treatment focuses on the underlying cause, not the antibody level itself.
- infections → treat the infection
- autoimmune disease → manage inflammation
- liver conditions → address liver health
- mild, temporary elevations → often need no treatment at all
Many people require only monitoring.
Daily life and self-care
Most people with polyclonal hypergammaglobulinemia can:
- continue normal daily activities
- monitor symptoms such as fever, joint pain, or fatigue
- manage liver or metabolic health if recommended
- follow their doctor’s guidance for follow-up tests
No diet restrictions or activity limits are required.
When should I call my doctor?
Call your doctor if you notice:
- fever
- unintentional weight loss
- night sweats
- persistent fatigue
- yellowing of skin or eyes
- new joint pain
- worsening liver test abnormalities
These symptoms help guide whether further evaluation is needed.
What is the usual plan going forward?
Most people need:
- periodic monitoring of immunoglobulin levels or SPEP
- follow-up liver tests if relevant
- evaluation of inflammation or infection if symptoms appear
Polyclonal hypergammaglobulinemia is common, stable, and often requires no specific treatment.
Making sense of it
Think of your immune system as a neighborhood full of helpful guard dogs. When something stirs — an infection, inflammation, or even long-standing medical conditions — many of these dogs bark at once. The noise is louder, not because anything dangerous is happening, but because the immune system is responding or has been active for a while.
A higher level of antibodies on your blood test often reflects this normal “background activity.” It doesn’t mean harmful cells are taking over. Instead, it usually signals that your immune system has been busy, recovering from illness, or reacting to chronic conditions like liver disease, autoimmune disorders, or inflammation.
Your doctor’s job is to understand why the immune system is more active and whether it fits a safe, expected pattern in your situation.
Key takeaways
- polyclonal hypergammaglobulinemia is usually benign and reflects immune activity
- it is different from monoclonal patterns, which behave differently
- most causes are common and relate to infection, inflammation, or liver health
- a bone marrow biopsy is rarely needed
- your doctor will guide follow-up based on the full clinical picture
For clinicians: Read our detailed guide on how to communicate about polyclonal hypergammaglobulinemia to patients.
