For Your Healthcare Provider
Have your patient scan this QR code with their smartphone camera to instantly access this educational guide on their device.

A guide for patients with elevated eosinophil counts
Access the Resources
Note: The video and audio linked above were generated with the assistance of AI. Clinical accuracy has been reviewed, but no AI-generated content can be guaranteed to be fully error-free.
A higher-than-expected eosinophil count is a common finding on routine blood tests.
In most cases, eosinophilia is related to everyday conditions such as allergies, asthma, or medications, and does not mean cancer or leukemia. Your doctor will help determine what is causing your result and whether any follow-up is needed.
This guide applies to outpatient evaluation and does not apply to emergency or rapidly worsening illness.
First things first
Eosinophils can increase for many everyday reasons, especially allergies, asthma, eczema, or medications. Many people with mild eosinophilia have no symptoms at all. A single higher reading does not usually mean something serious is happening.
What matters most is the overall picture: how high the count is, whether it is changing over time, and whether you have symptoms or related conditions. Your doctor will interpret your results in that broader context.
What are eosinophils?
Eosinophils are white blood cells involved in allergic responses, asthma, certain infections, and tissue inflammation.
Most eosinophils live in tissues such as the lungs, skin, and gastrointestinal tract. The blood test measures only the eosinophils passing through the bloodstream at the moment the sample was taken, which is why the number can change over time.
What is eosinophilia?
Eosinophilia means the eosinophil count is above the usual reference range on a complete blood count.
It is a finding, not a disease by itself. Mild eosinophilia is common and often relates to allergies, asthma, eczema, or medications. Most people with mild elevations have a clear explanation once symptoms, medications, and medical history are reviewed.
How eosinophils are measured
Your results may show:
- an absolute eosinophil count (the most useful number), or
- a percentage of eosinophils among white blood cells
The absolute count gives the clearest picture. Percentages can change when other white blood cells rise or fall, even if the eosinophil number itself has not changed.
Ranges that matter
Doctors often think about eosinophil levels in broad groups:
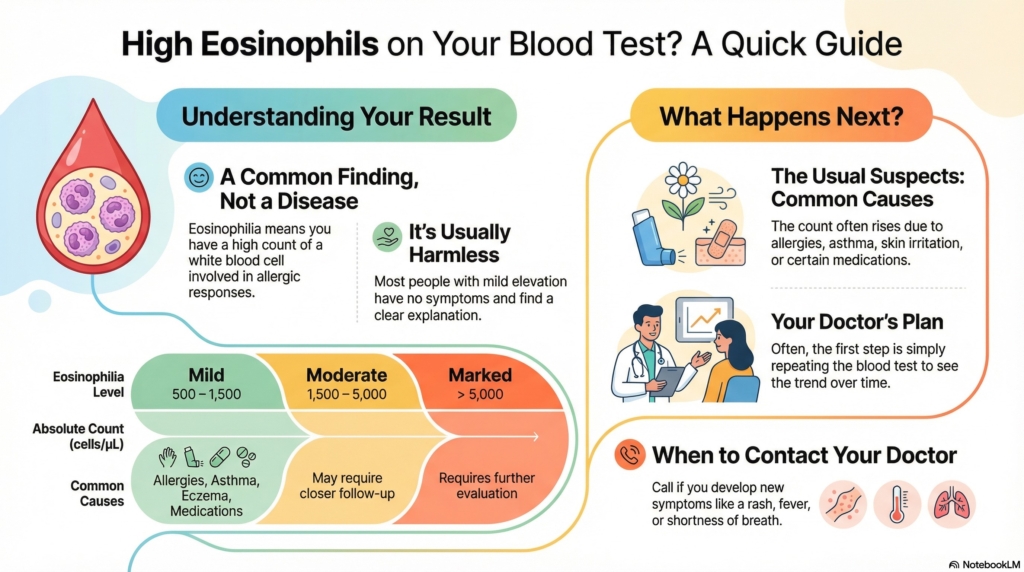
- mild eosinophilia (about 500–1,500 cells/µL or 0.5–1.5 x 109/L), most often related to allergies, asthma, eczema, or medications
- moderate eosinophilia (about 1,500–5,000 cells/µL or 1.5–5.0 x 109/L), which may need closer follow-up depending on symptoms
- marked eosinophilia (above 5,000 cells/µL or 5 x 109/L), which requires evaluation to understand the cause
These ranges are guides. Your doctor will interpret your results based on your symptoms, medical history, and overall health.
Why it happens (causes)
Eosinophils can rise for several reasons, including:
- common allergic conditions such as hay fever, asthma, or eczema
- medications, including some antibiotics, anti-inflammatory drugs, and other prescriptions
- skin irritation or inflammation
- seasonal triggers such as pollen exposure
- certain infections, especially when travel or specific exposures are relevant
- rarely, more complex immune or blood disorders
Your doctor will focus first on the most likely explanations based on how you feel and what is happening in your life. In some people, no single cause is identified and the pattern is simply monitored over time.
Does it cause symptoms?
Usually not. Most people with mild eosinophilia have no symptoms related to the eosinophil count itself.
When symptoms occur, they usually come from the underlying cause, such as allergy symptoms, asthma flare-ups, or skin itching. Eosinophilia itself does not cause fatigue or pain.
Is it dangerous?
For most people, eosinophilia is not dangerous. Mild or moderate elevations are usually related to allergies, asthma, medications, or temporary inflammation.
Rarely, very high eosinophil levels can affect organs such as the lungs, heart, skin, or nerves. This is uncommon and almost always occurs alongside clear symptoms, such as persistent rash, shortness of breath, or numbness.
Chronic eosinophilic conditions, such as hypereosinophilic syndrome, are rare and typically present with noticeable clinical problems rather than being found incidentally.
How your doctor evaluates it
Your doctor will review your symptoms, allergies, medications, travel or exposure history, and prior blood counts.
Often, the first step is simply repeating the CBC after a short interval to confirm the pattern. For mild elevations, this is commonly done after several weeks to a few months, for example after allergy season passes or a suspected medication is stopped.
Additional testing is usually ordered only if the eosinophil count remains high, increases over time, or if symptoms suggest a different condition. Most people find a clear explanation without needing extensive testing.
How is it treated
An elevated eosinophil count alone does not require treatment.
Care focuses on addressing the underlying cause, such as managing allergies or adjusting medications when appropriate. If you are concerned that a medication may be contributing, discuss this with your doctor before making any changes.
In rare conditions such as hypereosinophilic syndrome, treatment may include immune-modulating medications (such as steroids or targeted therapies) under specialist care.
Daily life and self-care
Most people with mild eosinophilia live normal, unrestricted lives.
Managing known allergies or asthma can help keep the eosinophil count stable. Seasonal changes may affect the level. No special diet, supplements, or activity limits are needed.
When should I contact my doctor?
Contact your doctor if you develop new or worsening symptoms such as:
- shortness of breath
- rash
- fever
- unexplained weight loss
- numbness, tingling, or muscle weakness
Also reach out if you miss a scheduled follow-up appointment, since tracking trends over time helps ensure the cause is understood.
What is the usual plan going forward?
Your doctor may repeat your blood count after weeks or months. If the eosinophil level returns to your usual range and you feel well, nothing further may be needed.
Many people have mildly elevated eosinophils throughout life without any health problems. Patterns over time are more important than a single number.
Making sense of it
Think of eosinophils as specialized cleanup crews that respond to allergens or irritation.
A slightly higher count usually means your body is reacting to something common, such as allergies, asthma, medications, or mild inflammation, not that a serious illness is present.
Key takeaways
- eosinophilia is a common finding, often related to allergies, asthma, or medications
- usually harmless, many people have no symptoms
- patterns over time matter, more than a single result
- treat the underlying cause, and the count often improves
- know when to call, new symptoms deserve evaluation
For clinicians: Read our detailed guide on how to communicate about eosinophilia to patients.
