For Your Healthcare Provider
Have your patient scan this QR code with their smartphone camera to instantly access this educational guide on their device.

A guide for patients with elevated basophil count
Access the Resources
Note: The video and audio linked above were generated with the assistance of AI. Clinical accuracy has been reviewed, but no AI-generated content can be guaranteed to be fully error-free.
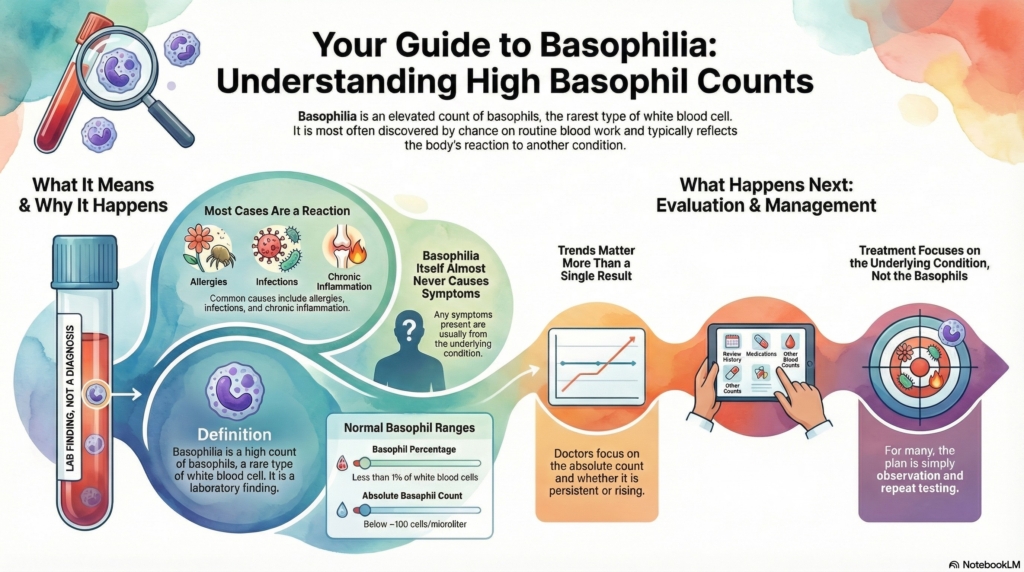
Basophilia means there are more basophils than usual in your blood test.
In most cases, this finding is mild, temporary, and related to allergies, inflammation, or another treatable condition.
This guide applies to outpatient evaluation and does not apply to emergency or rapidly worsening illness.
First things first
Basophils are the least common type of white blood cell. Because they are so rare, even a small change in their number can look noticeable on a blood test.
Most people with basophilia feel well. The finding is often discovered incidentally on routine blood work, rather than because it caused symptoms. Your doctor’s goal is to understand why the basophil count is elevated and whether it fits with your overall health, symptoms, and other blood results.
What are basophils?
Basophils are a rare type of white blood cell involved in immune signaling. They help coordinate responses to allergens and inflammation by releasing chemical messengers such as histamine.
Under normal circumstances, basophils make up less than 1% of all white blood cells. Because they are so uncommon, small changes in their number can appear more dramatic than changes in other white blood cell types.
Basophils are part of the body’s broader immune response system. They usually circulate quietly and are most active during allergic or inflammatory states.
What is basophilia?
Basophilia means there are more basophils than usual in the bloodstream on a blood test. It is a laboratory finding, not a diagnosis by itself.
Basophilia may be reported as:
- an increased absolute basophil count, or
- a higher percentage of basophils on the white blood cell differential
Doctors rely more on the absolute basophil count, because percentages can change when other white blood cells rise or fall.
In most cases, basophilia reflects a reaction to another process in the body, rather than a problem with the basophils themselves.
How basophils are measured
Basophils are counted as part of the complete blood count (CBC) with differential. The automated analyzer reports:
- the percentage of basophils among all white blood cells
- the absolute basophil count (ABC), calculated from the total white blood cell count and the basophil percentage
The absolute basophil count is the more reliable number when evaluating basophilia.
Ranges that matter
Basophils are normally present in very small numbers.
Most laboratories report:
- a basophil percentage of less than 1% of white blood cells
- an absolute basophil count that is typically below about 100 cells per microliter, though exact cutoffs vary by lab
Mild elevations are common and often temporary. A slightly high basophil percentage can occur even when the absolute count is normal, especially if other white blood cell types are lower.
Doctors focus most on the absolute basophil count and on trends over time, rather than on a single result.
Why it happens (causes)
Basophilia most often occurs as a reactive change, meaning it reflects something else happening in the body rather than a primary blood disorder.
Common causes include:
- infections
- chronic inflammation or autoimmune conditions
- allergies or allergic conditions
- medication effects
- recovery after illness, stress, or surgery
Less commonly, persistent or marked basophilia, especially when accompanied by other abnormal blood counts, may be associated with bone marrow or blood disorders, including certain myeloproliferative neoplasms.
Context matters. Your doctor interprets basophilia alongside symptoms, other blood counts, and how the values change over time.
Does it cause symptoms?
Basophilia itself almost never causes symptoms.
When symptoms are present, they usually come from the underlying condition causing the basophil count to rise. These may include:
- allergy-related symptoms
- signs of infection or inflammation
- symptoms related to other blood count abnormalities
Many people learn they have basophilia only because it appeared on routine blood work.
Is it dangerous?
In most cases, no.
Mild or temporary basophilia is usually harmless. Concern increases when basophilia is:
- persistent over months,
- rising over time, or
- accompanied by other abnormal blood counts or new symptoms
Your doctor’s role is to distinguish common, benign causes from less common conditions that need closer evaluation.
How your doctor evaluates it
Evaluation is guided by the overall clinical picture, not by a single number.
Your doctor may:
- review symptoms, allergies, medications, and medical history
- repeat blood tests to look for trends
- examine the rest of the white blood cell differential
- look for signs of infection, inflammation, or endocrine conditions
Additional testing is usually reserved for cases where basophilia is persistent, unexplained, or accompanied by other concerning findings.
How is it treated
There is no treatment directed at basophils themselves.
Management focuses on:
- treating any identified underlying condition,
- monitoring blood counts over time, or
- addressing a bone marrow disorder if one is found.
In many cases, no treatment is needed.
Daily life and self-care
Basophilia usually does not require lifestyle changes.
Helpful steps may include:
- managing known medical conditions as advised by your doctor.
- taking medications as prescribed.
- keeping follow-up appointments for repeat testing.
Most people can continue normal daily activities.
When should I contact my doctor?
Contact your doctor if you develop new or worsening symptoms, including:
- unexplained fevers, night sweats, or weight loss.
- abdominal fullness or early satiety.
- new abnormalities on repeat blood tests.
If you feel well and your doctor has recommended monitoring, it is reasonable to wait for scheduled follow-up.
What is the usual plan going forward?
For many people, the plan is observation and reassurance.
This often includes:
- repeating the blood count after time has passed,
- watching trends rather than reacting to a single result,
- addressing any identified underlying condition.
Only a small minority of patients require extensive testing or long-term follow-up.
Making sense of it
Basophils are like rare messengers in the immune system. Because there are so few of them, small changes can look dramatic on paper.
Most of the time, basophilia is the body’s way of signaling a temporary or manageable condition, rather than something dangerous.
Key takeaways
- basophilia is a high basophil count, often found incidentally on blood tests
- most mild elevations are temporary, related to infections, inflammation, medications, or other common conditions
- basophilia itself causes no symptoms, though the underlying cause may
- persistent or marked elevations, especially with other abnormal blood counts, may warrant specialist evaluation
- trends over time matter more than a single result, and care focuses on identifying the underlying cause
For clinicians: Read our detailed guide on how to communicate about basophilia to patients.
