For Your Healthcare Provider
Have your patient scan this QR code with their smartphone camera to instantly access this educational guide on their device.

A guide for patients with low hemoglobin
Access the Resources
Note: The video and audio linked above were generated with the assistance of AI. Clinical accuracy has been reviewed, but no AI-generated content can be guaranteed to be fully error-free.
Anemia is a common finding on blood tests.
In many cases, it is mild, temporary, and treatable.
Anemia is not a diagnosis by itself. It is a signal that helps doctors decide whether further evaluation or monitoring is needed.
Most people with anemia do not have a serious underlying condition, especially when other blood counts and symptoms are reassuring.
This guide applies to outpatient evaluation and does not apply to emergency or rapidly worsening illness.
First things first
Not all anemia is the same.
Doctors do not evaluate anemia based on a single number or a single cause. Instead, they look at patterns in blood tests, symptoms, and medical history to understand why anemia is present.
Small changes in hemoglobin are common and do not always require treatment. What matters most is the overall pattern and how it changes over time.
What is anemia?
Anemia means that the blood has a reduced ability to carry oxygen.
Doctors identify anemia using hemoglobin and hematocrit, which reflect how much oxygen-carrying capacity is present in the blood. When these values are low, anemia is present.
Although it may seem intuitive to use the red blood cell count to define anemia, doctors do not rely on this number. Instead, they use hemoglobin and hematocrit, which are better measures of how well the blood can deliver oxygen to the body.
Anemia is commonly defined using hemoglobin thresholds. For non-pregnant adults, hemoglobin levels below 12 g/dL in women or 13 g/dL in men are often used to define anemia.
These cutoffs are guides rather than absolutes. Doctors interpret them alongside symptoms, trends over time, and the individual clinical context.
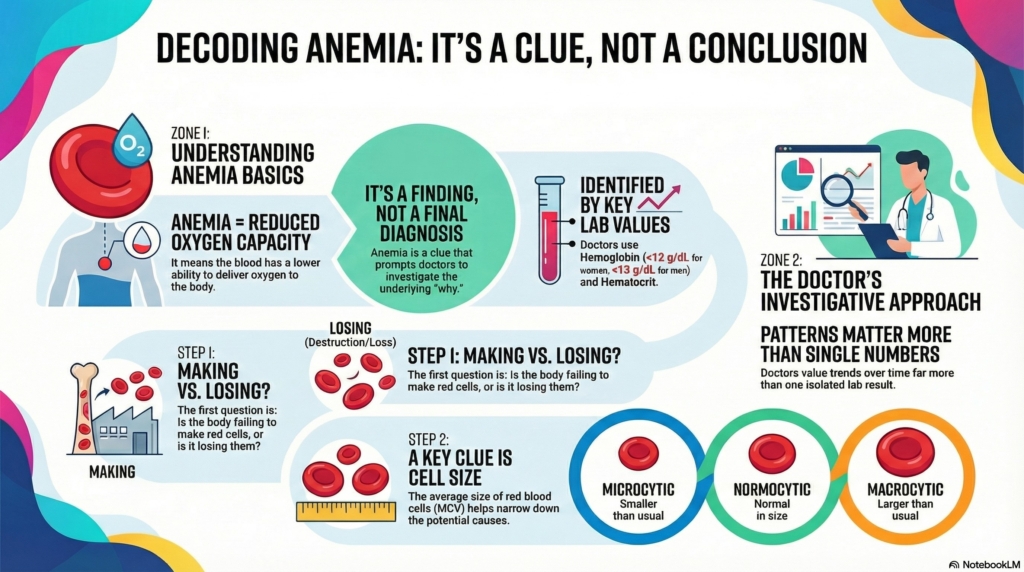
Anemia itself is a finding, not a diagnosis. It does not explain the cause. Instead, it prompts the next question: why is this happening?
Different conditions can lead to anemia, and the approach depends on understanding the underlying process rather than reacting to the number alone.
How doctors begin to think about anemia
When anemia is present, doctors first ask two broad questions:
- Is the body losing or destroying red blood cells, or
- Is the body not making enough red blood cells?
To help answer this, doctors use additional information from the blood count and, in some cases, other tests. These patterns help narrow the possibilities and guide further evaluation.
Red blood cell size and anemia
One of the most helpful clues comes from the mean corpuscular volume (MCV), which reflects the average size of red blood cells.
Based on red cell size, anemia is often grouped into three broad patterns:
- microcytic anemia, where red blood cells are smaller than usual
- normocytic anemia, where red blood cells are normal in size
- macrocytic anemia, where red blood cells are larger than usual
These categories do not make a diagnosis, but they help doctors decide which causes are more or less likely.
Anemia can exist with or without symptoms
Some people with anemia feel well, especially when the anemia is mild or develops slowly. The body can often adapt to gradual changes in hemoglobin.
Others may notice symptoms such as fatigue, shortness of breath, dizziness, or reduced exercise tolerance. Symptoms depend on how low the hemoglobin is, how quickly it changed, and the person’s overall health.
Doctors consider symptoms alongside lab results when deciding next steps.
Snapshot vs movie
A blood test shows anemia at one moment in time.
Doctors place far more weight on trends over time than on a single result. This is why repeat testing is common and often reassuring.
A stable pattern is usually more important than an isolated abnormal value.
How this page fits with the rest of your results
This page explains how doctors think about anemia in general.
If anemia is present, your doctor may point you to more focused information on topics such as:
- microcytic anemia
- normocytic anemia
- macrocytic anemia
- iron deficiency or other specific causes
Each of those builds on the same principles outlined here.
Key takeaways
- what anemia means: reduced oxygen-carrying capacity of the blood
- how it’s identified: hemoglobin or hematocrit, not red cell count alone
- what it is not: anemia is a finding, not a diagnosis
- how doctors interpret it: patterns matter more than single numbers
- why follow-up helps: trends over time guide decisions
For clinicians: Read our detailed guide on how to communicate about anemia to patients.
