Livedo reticularis
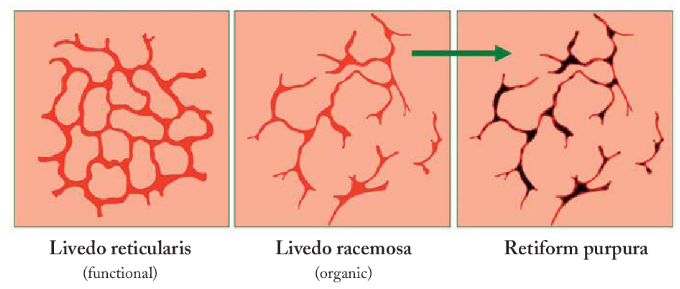
On the patient’s skin exam, you note branching, netlike, mottled purpuric lesions, consistent with livedo reticularis. This finding is caused by perfusion defects in the underlying vasculature, producing localized cyanosis at the site of blood vessel.
Contrast this with retiform purpura (seen in calciphylaxis, vasculitis, or hypercoagulable states such as warfarin skin necrosis or disseminated intravascular coagulation [DIC]). Retiform purpura is similarly comprised of netlike purpuric lesions due to underlying vascular disturbances; however, retiform purpura is a reflection of severe perfusion deficits resulting in tissue necrosis and ulceration (not just cyanosis, which is theoretically reversible with if perfusion improves).
As livedo reticularis reflects temporary disturbances in skin oxygenation, it is not unique to cold agglutinin disease; it can occur due to a number of underlying processes as listed below.
- Obstructive vasculopathies: eg. hypercoagulable states (DIC, antiphospholipid syndrome), cold agglutinin disease, cryoglobulinemia
- Inflammatory/vasculidities: granulomatosis with polyangiitis (GPA), polyarteritis nodosa, thromoboangiitis obliterans, lupus, rheumatoid arthritis
- Infectious: disseminated bacterial infection (eg. meningococcal or streptococcal bacteremia, septic emboli), hepatitis C infection
- Drug-associated: catecholamine pressors, NSAIDs
- Malignant infiltration: mycosis fungoides, inflammatory breast cancer