How expert consultants define terrain, assign weight, and make judgment visible when laboratory markers suggest red cell destruction and stakes are real
Note: The video and audio linked above were generated with the assistance of AI. Clinical accuracy has been reviewed, but no AI-generated content can be guaranteed to be fully error-free.
More Than a Pattern: How Expert Consultants Manage Suspected Hemolysis
Laboratory markers that suggest hemolysis often appear striking.
But the danger in suspected hemolysis is rarely the lab pattern alone.
The same constellation of findings — falling hemoglobin, elevated LDH, indirect hyperbilirubinemia, low haptoglobin — can live in very different clinical worlds.
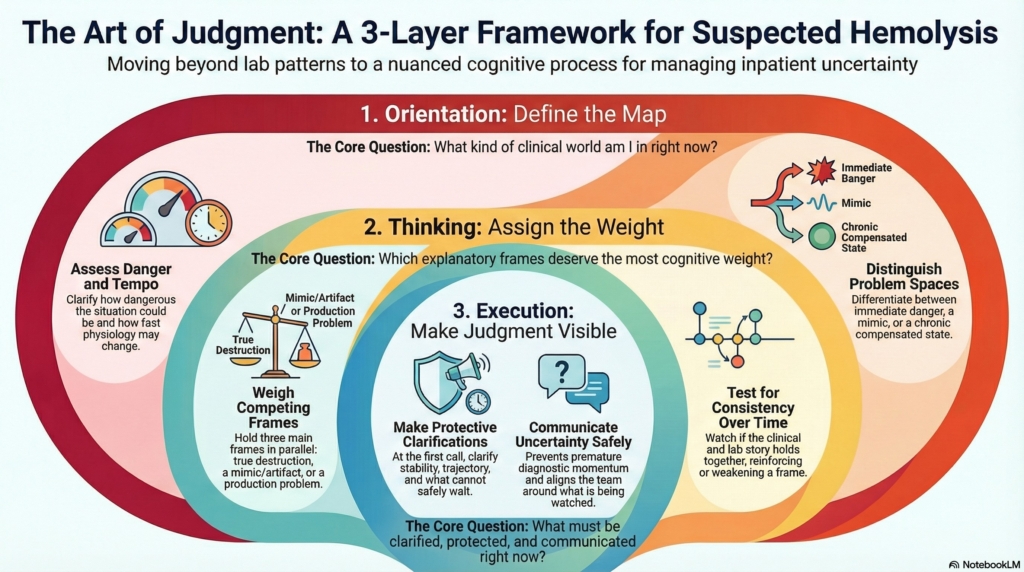
This graphic shows how expert consultants use a three-layer framework — Orientation, Thinking, and Execution — to define terrain, assign cognitive weight, and make judgment visible in real clinical time.
Rather than rushing to label a cause, this approach prioritizes danger, tempo, and internal consistency, helping clinicians manage uncertainty safely and avoid premature diagnostic momentum.
Why suspected hemolysis is a consult problem, not a lab problem
In hospitalized patients, suspected hemolysis is rarely just a laboratory abnormality.
It is a signal — of physiologic reserve, systemic illness, evolving risk, and potential misinterpretation.
The same laboratory pattern can mean very different things in different patients:
- a patient with chronic compensated hemolytic anemia
- a septic patient with inflammatory marker elevation mimicking hemolysis
- a patient with true acute red cell destruction
- a patient with marrow suppression and misleading turnover markers
- or a patient with transfusion-related or systemic stress artifacts
In each case, the pattern may look similar.
The danger is not.
This is why suspected hemolysis is not primarily a diagnostic problem.
It is a judgment problem.
Expert consultation is not about naming a mechanism as quickly as possible.
It is about safely managing uncertainty, defining risk, and adapting posture as biology declares itself.
Consult Practice makes that expert judgment visible.
The three-layer framework: Orientation, Thinking, Execution
This series approaches suspected hemolysis through three distinct cognitive layers:
- Orientation — defining the terrain
- Thinking — assigning weight within that terrain
- Execution — making judgment visible through action and communication
Each layer has a different job.
Confusing them is one of the most common sources of clinical error.
Orientation defines the map
Orientation answers a simple but powerful question:
What kind of clinical world am I in right now?
Orientation is not diagnosis.
It is terrain definition.
In suspected hemolysis, Orientation clarifies:
- how dangerous this situation could be
- how fast physiology may change
- how much uncertainty can be safely tolerated
- and whether this pattern likely reflects true destruction, a mimic, or a chronic/compensated state
Orientation emphasizes the tempo × threat map:
- acute + unstable worlds
- acute but stable evolving worlds
- chronic compensated worlds
- and ambiguity worlds that require surveillance
Orientation helps distinguish between terrains such as:
- immediate physiologic danger
- plausible destruction requiring vigilance
- chronic compensated anemia
- multi-process systemic or marrow-limited states
- laboratory mimic or artifact patterns
These are not causes.
They are problem spaces.
Orientation often begins at the time of the page, but it is not a one-time act.
Whenever new information changes the nature of the situation, Orientation is re-invoked.
Orientation answers:
What kind of situation is this?
Thinking assigns weight within the defined world
Once the terrain is defined, Thinking takes over.
Thinking answers a different question:
Within this world, which explanatory frames deserve the most cognitive weight right now?
In suspected hemolysis, Thinking is not about choosing a diagnosis.
It is about weighting competing frames:
- destruction-dominant frames
- mimic or artifact frames
- production-limited or systemic suppression frames
Thinking focuses on:
- trajectory
- internal consistency
- clinical coherence
- and consequence if the weighting is wrong
Expert consultants:
- hold multiple frames in parallel
- increase or decrease vigilance as biology declares itself
- resist premature mechanistic labeling
- and release concern when consistency weakens
Thinking is where consultants protect against:
- over-calling hemolysis based on a single snapshot
- anchoring on striking but nonspecific markers
- and forcing unification before the story holds together
Thinking answers:
Which frames deserve the most attention right now, and what would change that?
Execution makes judgment visible
Execution is where judgment becomes real to others.
Execution answers:
What must be clarified, protected, communicated, deferred, and revisited — right now?
This is where:
- physiologic safety is protected
- monitoring is prioritized
- uncertainty is communicated
- and reassessment is made explicit
Execution is not running a hemolysis checklist.
It is translating judgment into safe clinical behavior over time.
Execution includes:
- first protective clarifications
- tempo-based reassessment
- visible restraint when appropriate
- protective escalation when necessary
- and transparent recalibration as biology evolves
This is why Execution is best described as:
Judgment made visible.
Execution answers:
How does expert judgment look in real clinical time?
Why this framework matters
Many errors in suspected hemolysis do not arise from lack of knowledge.
They arise from:
- treating lab patterns as diagnoses
- over-weighting nonspecific markers
- confusing mimic with destruction
- forcing early mechanistic closure
- or failing to adapt posture as trajectory evolves
This framework protects against category failure:
- treating ambiguity like a diagnostic puzzle
- treating evolving physiology like a static abnormality
- treating uncertainty as something to eliminate rather than manage
By separating Orientation, Thinking, and Execution, the consultant:
- defines the correct terrain
- assigns weight deliberately
- and makes judgment visible and adaptable
This is how expert consultants manage risk when facts are incomplete and stakes are real.
How to use this series
This overview is the conceptual front door.
The three companion essays go deeper:
- Orientation — for defining the problem space
- Thinking — for frame-weighting under uncertainty
- Execution — for visible action and communication over time
They are designed to be used together.
Not as algorithms.
Not as diagnostic manuals.
But as a guide to how expert consultants think, act, and recalibrate in real clinical environments.
Bottom line
Suspected hemolysis in hospitalized patients is not a diagnosis.
It is a signal.
Expert care depends on:
- defining what kind of world the patient is in
- assigning cognitive weight within that world
- and making judgment visible through safe, adaptive execution
Orientation defines the map.
Thinking assigns weight.
Execution makes judgment visible.
That is how hematologists reason when laboratory markers suggest hemolysis and the stakes are real.
