CASE OF THE WEEK
When a disease stops behaving like itself
Learning objectives
By the end of this case, you should be able to:
- recognize change in tempo as a key signal of altered disease biology
- distinguish CLL progression from Richter transformation based on clinical, laboratory, and imaging features
- identify discordant findings (focal mass, high LDH, stable CBC) that suggest transformation
- understand the limitations of peripheral blood and imaging in defining disease identity
- interpret immunophenotypic shifts (e.g., CD20 loss, CD23 loss, high Ki-67) in aggressive lymphomas
- explain why tissue diagnosis is required when disease behavior changes
Opening vignette
A 79-year-old woman with a long history of chronic lymphocytic leukemia presents with several days of worsening abdominal fullness and right upper quadrant pain.
She describes a growing “mass-like” sensation.
She has been clinically stable with slowly progressive CLL for years.
Now, the rate of change is different.
What is the most important feature of this presentation?
Teaching point:
When a chronic disease changes tempo, reassess the underlying biology.
History of present illness
- Progressive RUQ pain over several days
- Worse with movement
- Decreased appetite
- No fevers, chills, or night sweats
- No nausea, vomiting, or diarrhea
What is the differential diagnosis for this patient?

Sort the following into categories:
Teaching point:
At this stage, the task is not to name the diagnosis, but to frame the problem broadly.
In a patient with known CLL and this tempo of change, what type of process is most concerning?
Teaching point:
A change in tempo should prompt the question:
What kind of disease is this now?
Additional history
Five months earlier:
- Presented with abdominal pain
- Found to have biliary obstruction
- Underwent ERCP with stent placement
- Biopsy at that time was inconclusive
- Symptoms resolved completely
How should this prior episode influence your thinking?
Reflection
Looking back, the prior episode of biliary obstruction is a warning.
Biliary obstruction is unusual in indolent CLL.
A focal obstructive process in this setting suggests a structural lesion and may represent an early manifestation of transformation.
CLL history
- Diagnosed years earlier
- Treated with chlorambucil, later pentostatin/cyclophosphamide/rituximab
- Gradual progression over time
- Recent lymph node biopsy:
→ CLL with scattered paraimmunoblasts
Physical exam
- Palpable right upper quadrant mass (~6–7 cm)
- No significant peripheral lymphadenopathy
What is most notable about this exam?

Match each finding to its interpretation:
Teaching point:
Transformation is often biochemically loud but hematologically quiet.
Imaging
CT scan shows:
- Large heterogeneous right upper quadrant mass
- No widespread bulky lymphadenopathy
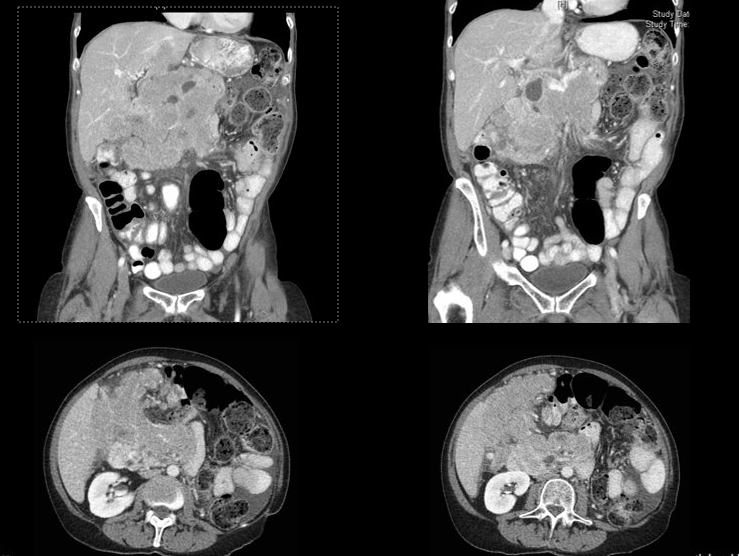
What does this imaging pattern suggest?
Biopsy (initial findings)
- Large atypical cells
- Negative for CD20
- Negative for CD3
CT-guided Core Needle Biopsy of Abdominal Mass
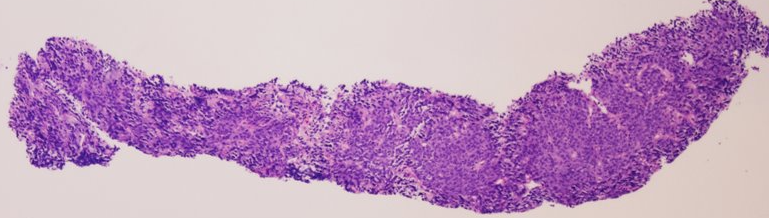
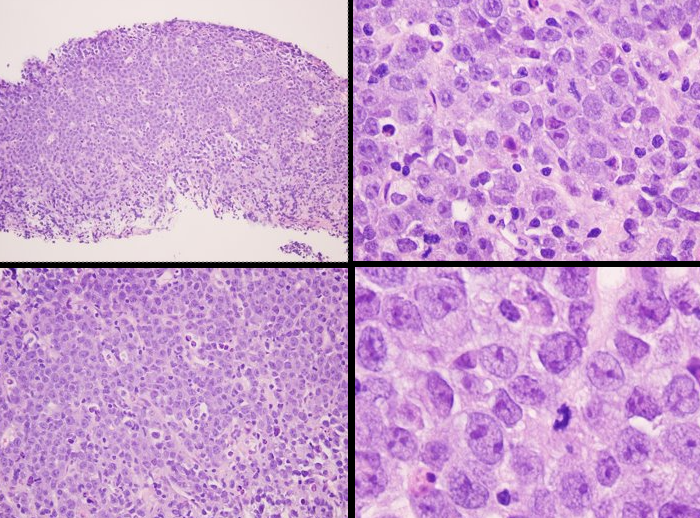
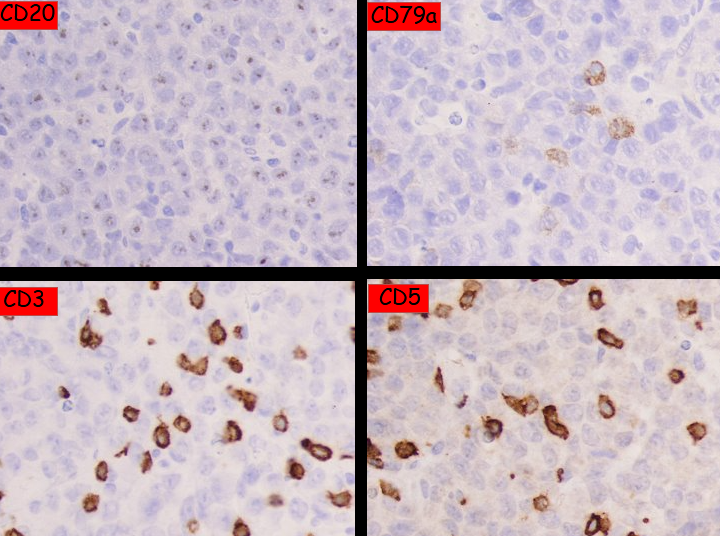
What do you make of the biopsy and immunoperoxidase findings?
Interpretation
Loss of lineage markers creates diagnostic uncertainty.
CD20 negativity does not exclude B-cell lymphoma
→ may occur after prior therapy or in aggressive disease
What is the next best step to secure a definitive diagnosis?
Additional studies
- PAX5 positive
- Ki-67 high
- CD23 negative
What do these findings indicate?

Sort the following features:
Diagnosis
The mass represents a high-grade B-cell lymphoma (diffuse large B-cell lymphoma) arising in a patient with known CLL.
This is Richter transformation.
What is Richter transformation?
Richter transformation refers to the development of an aggressive lymphoma in a patient with chronic lymphocytic leukemia.
- most commonly transforms to diffuse large B-cell lymphoma (DLBCL)
- less commonly to Hodgkin lymphoma
- represents a change in disease biology, not simply progression
- typically presents with rapid clinical deterioration, focal mass, and elevated LDH
- often arises through clonal evolution of the original CLL, though some cases represent a second, unrelated lymphoma
How would you treat this patient?
Treatment framework
- treat as aggressive lymphoma (DLBCL)
- regimens such as R-CHOP or equivalent
- consider clinical trials
- prognosis worse than CLL
Key insight
When tempo, distribution, and laboratory signals become discordant, reconsider the diagnosis.
Closing reflection
Chronic diseases teach us patterns.
Transformation breaks them.
The challenge is not recognizing what fits.
It is recognizing when something no longer does.

